Longevity and Health Span Blog
Author Jonathan A. Jarman, MD is a Yale–NYU trained physician engaged in health-optimization and longevity research. His work focuses on the physiology of high-performance aging, including VO₂max, muscle strength, autonomic regulation, emotional control, and cognitive resilience. He leads the Julian A. Jarman MD Research Foundation, which supports and advances research in these domains.
5 Part Series - Myths, Lies & Truths about Testosterone & Anabolic Steroids
Intro: Myths, Lies & Truths About Testosterone & Anabolic Steroids
This blog will be released in 5 parts over 4-5 weeks:
Introduction
- Part 1: The History of Anabolic Steroids
- Part 2: Why the Fear Around Anabolic Steroids?
- Part 3: Testosterone Analogs
- Part 4: Testosterone alternatives (SARM), Clomid, hCG, GnRH
Understanding Testosterone, Anabolic Steroids, and the Science Behind Hormone Replacement Therapy (HRT)
Misinformation about testosterone and its synthetic analogs (anabolic steroids/AAS) is widespread. Surprisingly, even scientific literature has contributed to this confusion. Over 50 years ago, two published studies claimed that AAS had no impact on muscle growth (23,24).
However, these early studies were methodologically flawed—using low dosages, short durations, and inadequate resistance training protocols. Did the researchers have an agenda, designing their studies to produce a predetermined outcome? Possibly. Regardless of intent, these misleading and incorrect conclusions were later disproven by well-designed studies in the 1980s and beyond.
When Science Gets It Wrong
How is it possible for science to be wrong? After all, weren’t we urged during the COVID-19 pandemic to “Follow the science”? The reality is that not all scientific studies are created equal.
Poorly designed studies with flawed conclusions exist and often fail replication—a critical test of scientific validity. In an essay published in PLoS Medicine / August 2005 | Volume 2 | Issue 8, Stanford University professor John Ioannidis, PhD wrote, “There is increasing concern that in modern research, false findings may be the majority or even the vast majority of published research claims. (25,26).
The vitriol against Ioannidis on his views and research during the COVID-19 pandemic was severe as many scientists refused to consider another, and different, analysis of the data because it opposed their politically driven agenda. More and more, we are seeing the aggressive suppression of science and analysis of data that does not agree with a particular political group.
The phrase “Follow the science” was often misused to mean “Follow the science that aligns with our particular agenda.” It was used to manipulate behavior. A more accurate principle would be:
“Follow the good science, not the bad science.” Importantly, even good science evolves as new knowledge emerges.
Balancing Risks and Benefits
All medications have a risk-to-reward ratio, and higher doses and improper use increase the risks significantly. Testosterone and its synthetic analogs are no exception.
- When properly prescribed and monitored by a knowledgeable physician, their benefits can be transformative.
- When misused or abused without medical supervision, the risks can become severe, even life-threatening.
The Purpose of This Blog
This blog aims to be a definitive resource on hormone replacement therapy (HRT), covering both testosterone and its synthetic analogs.
A comprehensive review of the scientific literature on male HRT and recreational use was conducted for this blog, though it remains an evolving field. Over 50 papers were identified and analyzed using search terms such as: testosterone, anabolic steroids, HRT, history of testosterone synthesis, erectile dysfunction, Deca-Durabolin, nandrolone and many others.
At the Julian A. Jarman, MD Research Foundation, a non-profit Men’s Health Foundation, understanding HRT, testosterone, and its analogs is a core priority. Providing accurate, science-backed information empowers men to make informed decisions about their health.
Part 1: Myths, Lies & Truths About Testosterone & Anabolic Steroids
Part 1: The History of Anabolic Steroids
Understanding Testosterone and Anabolic Steroids
First it is important to understand that testosterone is an anabolic steroid. Both testosterone and its synthetic analogs fall under the category of androgenic anabolic steroids (AAS). While the term “anabolic steroids” often refers to synthetically manufactured drugs, all AAS originate from testosterone or its metabolites. Going forward, I will use AAS to refer to both testosterone and its synthetic analogs as a single group of male hormones.
Both testosterone and its synthetic analogs are derived from cholesterol, which serves as the precursor to all male and female hormones. In men, the testes primarily produce testosterone, while in women, smaller amounts of testosterone are synthesized in the ovaries and adrenal glands. Despite cholesterol’s negative connotation and its association with heart disease in excessive amounts, cholesterol is essential for life. We make our own cholesterol and there is is no “essential minimum” LDL-cholesterol needed in your blood to make male and female hormones, cortisol and Vitamin D, which are all synthesized from cholesterol. Despite concerns of some regarding driving LDL-cholesterol too low, current evidence supports that LDL-C levels < 20-30 mg/dL are safe and do not compromise the body’s ability to produce hormones or other essential cholesterol-derived molecules. (30)
Most commercially produced testosterone today comes from plant sterols extracted from yams and soybeans, as this method is both efficient and cost-effective. Although other production methods exist—such as direct cholesterol conversion and microbial *transformation*—they are less commonly used in industrial applications. This plant-derived testosterone is identical to the body’s natural hormone and is often referred to as a “bioidentical hormone.”
Why Create Testosterone Analogs?
Testosterone analogs—what most people associate with the term anabolic steroids— are chemically modified versions of testosterone. These modifications enhance anabolic (anabolic means muscle-building) effects while aiming to reduce androgenic (androgenic means masculinizing) side effects.
Well-known AAS include:
- Nandrolone (Deca-Durabolin)
- Methandrostenolone (Dianabol)
- Oxandrolone (Anavar)
- Stanozolol (Winstrol)
- Boldenone (Equipoise)
Each of these compounds has unique properties, which we will discuss later.
The Role of Testosterone in Both Sexes
Both men and women need testosterone for:
- Sexual development and reproduction
- Muscle and bone health
- Cognitive function
Testosterone is also the precursor to estrogen. While women naturally produce much lower levels than men, testosterone remains vital to their overall health.
The Misinformation About Anabolic Steroids
Misinformation about AAS has been—and continues to be—spread by both medical professionals and the general public. As noted in the introduction, in the 1960s and 1970s, some researchers claimed that AAS did not increase muscle mass, relying on poorly designed studies (23,24).
Today, however, there is no debate—testosterone and its analogs unequivocally enhance muscle growth.
Why Were Testosterone Analogs Created?
If testosterone is so effective, why did pharmaceutical companies develop synthetic analogs? The answer lies in the anabolic-to-androgenic ratio of each compound.
- Anabolic effects promote muscle growth.
- Androgenic effects contribute to masculinization (e.g., body hair growth, scalp hair loss, deepening voice, increased aggression, and genital enlargement in women).
The goal was to create *a male hormone with stronger anabolic effects and fewer androgenic side effects*—leading to the development of synthetic AAS for medical use that could be used for both men and women with various medical problems.
Anabolic Steroids Were Created to Treat Disease
Despite their association with athletes and bodybuilders, anabolic steroids were originally developed to treat medical conditions such as:
- Anemia
- Osteoporosis
- Severe weight loss and muscle-wasting diseases
- Hypogonadism (low testosterone production)
- Delayed puberty
For full disclosure, I was personally treated with the AAS Stanozolol (Winstrol) for delayed puberty.
Since their creation in the 1930s, AAS have proven valuable for many other medical applications.
The First Anabolic Steroids
- 1935 – Scientists successfully synthesized testosterone for the first time.
- 1950s – The first widely recognized AAS, Methandrostenolone (Dianabol), was synthesized by CIBA Pharmaceuticals.
- Dianabol’s advantage over testosterone? It was indeed more anabolic and less androgenic, as desired in its synthesis, marking the beginning of efforts to create steroids that build muscle with fewer masculinizing effects.
This was a major advancement—developing a testosterone derivative that treated certain diseases, enhanced muscle growth while reducing unwanted side effects so it could be used for both men and women.
Steroid Use in Sports & Bodybuilding
By the 1950s, AAS use had expanded beyond medical treatments into performance enhancement.
- 1954 – The Soviet Union dominated the World Weightlifting Championships, later revealed to be due to testosterone use.
- 1960s – AAS use exploded in bodybuilding and competitive sports.
1965 – The first Mr. Olympia competition was held, and AAS use became common among professional bodybuilders.
Today, it is highly unlikely that any professional bodybuilder competes without using AAS. In fact, even Arnold Schwarzenegger has admitted to using anabolic steroids.
Part 2: Myths, Lies & Truths About Testosterone & Anabolic Steroids
Part 2: Why the Fear Around Anabolic Steroids?
Why the Fear Around Anabolic Steroids?
It has been said that there are greater negative views for anabolic steroid use than opioid abuse, despite the fact that opioid addiction has caused a significant public health crisis and AAS has not. While both anabolic steroids and opioids have risks, AAS’s are not linked to overdose deaths like with opioids. Yet AAS carry a greater social stigma—especially in professional sports where their use is banned. Meanwhile, opioid addiction is viewed as a medical and mental health problem leading to a more compassionate response despite its devastating impact.
Despite their medical benefits, anabolic steroids are often demonized. Why?
This fear is largely driven by:
- Misinformation spread by both medical professionals and the media.
- Association with cheating in sports serious health risks.
- Association with cheating in sports rather than their legitimate medical applications.
AAS are not inherently dangerous—when used correctly under knowledgeable medical supervision. However, like any powerful medication, misuse can lead to serious consequences.
In the next section, we’ll explore the benefits, risks, and misconceptions surrounding AAS use.
In 2023, the CDC reported over 81,000 opioid-related deaths (1). In contrast, the relationship between anabolic androgenic steroid (AAS) use and mortality is far less clear. Many reported cases of AAS-related deaths involve *polypharmacy*—the concurrent use of multiple substances—making it difficult to isolate anabolic steroids as the sole cause of death.
A 2024 study published in The New England Journal of Medicine, titled “Higher Mortality is Associated with Anabolic Steroid Use” (2), found that AAS users have a 2.8 times higher risk of death than non-users. However, it is crucial to distinguish correlation from causation. While these findings suggest a link between AAS use and increased mortality, confounding factors make it difficult to establish a direct causal relationship. Furthermore, comprehensive and up-to-date statistics on deaths solely attributed to anabolic steroids remain limited.
To be clear, my intent is not to downplay the potential risks of AAS use and abuse. Rather, I emphasize that *data on AAS-related deaths is scarce*—especially when compared to mortality from tobacco, alcohol, or opioids.
All Drugs Have a Risk-to-Reward Ratio
Every drug—whether prescription medication, food, supplements or even oxygen—carries both risks and benefits. Oxygen is essential for life, yet excessive oxygen exposure can damage the lungs and be fatal. The same principle applies to *AAS and all medications*—their impact depends on dosage, duration, and medical supervision.
When used under careful medical oversight, AAS can:
- Enhance performance
- Increase lean muscle mass
- Reduce body fat
- Improve cholesterol levels
The widespread fear of AAS use is largely unfounded when they are used responsibly under medical guidance. Later in this blog, we will explore the benefits of testosterone and its analogs in greater detail.
The Risks of AAS Use
Using anabolic androgenic steroids (AAS) without medical supervision carries serious health risks, including potentially fatal consequences. However, when prescribed and monitored by a knowledgeable physician, these risks can be minimized and managed effectively.
Many articles present long, alarming lists of AAS risks, misleading the public into believing that all listed side effects are equally likely. The reality is *far more nuanced—risk levels depend on dosage, duration, individual genetics, and whether proper post-cycle therapy (PCT) is implemented. Additionally, the specific AAS used also plays a critical role in side effect severity.
When testosterone replacement therapy (TRT) is administered at physiologic doses—meaning it restores testosterone levels to a natural, healthy range—its impact on biomarkers is generally predictable and manageable.
However, even at physiologic doses, some biomarkers can be influenced. Let’s break down the most commonly cited risks for biomarkers, other side effects and vital signs:
1. “Roid Rage” – Aggression & Mood Changes
At physiologic doses, AAS enhance mood and can increase confidence and motivation. However, at high doses, they disrupt neurotransmitter balance, increasing aggression:
- Increased dopamine → Heightened reward-seeking behavior and impulsivity.
- Decreased serotonin → Lower impulse control, increasing irritability and aggression. (19, 20)
2. Acne
A well-documented side effect, acne worsens with higher doses. However, women are more prone to AAS-induced acne than men due to hormonal sensitivity. (18)
3. Hair Loss (Male Pattern Baldness)
AAS accelerate hair loss only in individuals genetically predisposed to male pattern baldness. This is due to increased dihydrotestosterone (DHT) levels, which can be mitigated with 5α-reductase inhibitors like finasteride.
4. Cardiovascular Risks
Medical opinions on testosterone replacement therapy (TRT) and heart health have reversed course over the last decade.
- In 2010, a study prematurely halted TRT due to an alleged increase in cardiovascular (CV) risk. (21)
- Public Citizen, an advocacy group, petitioned the FDA for a black box warning on testosterone, but the FDA rejected it, citing an equivocal causal relationship between TRT and heart disease.
- Newer research, including a 2023 New England Journal of Medicine study, tracking 5,200 men aged 45–80, found no increased risk of heart attack or stroke with TRT use. (22)
Biomarkers of importance:
Total Testosterone (Range: 400–1,000 ng/dL) (Note that laboratories have slightly different ranges.
- Goal: Maintain levels within an optimal physiological range
Free Testosterone (Range: 10–30 pg/mL)
- Measures active testosterone (more relevant than total T)
- Influenced by SHBG levels- too high reduces free testosterone.
- SHBG reduction means to increase free T include: increasing resistance training, increase protein intake, optimize thyroid, take Zine and Magnesium
Estradiol (Ideal: ~20–40 pg/mL)
- Too high → Water retention, gynecomastia (male breast tissue growth), mood swings, breast tenderness
- Too low → Joint pain, fatigue, low libido
- Managed with AI (aromatase inhibitors) if necessary, but overuse can be harmful
- Using testosterone cream tends to reduce this issue vs injected testosterone!!
Hemoglobin/Hematocrit
- T can increase red blood cell (RBC) production
- Too high → Risk of blood thickening (polycythemia), high blood pressure, stroke, cardiovascular risks
- Managed by donating blood (therapeutic phlebotomy) or adjusting dose
Prostate-Specific Antigen (PSA) (Ideal: <4.0 ng/mL)
- TRT doesn’t cause prostate cancer, but monitoring PSA ensures early detection of abnormalities
- Significant increase → Further evaluation needed
Lipid Panel (Cholesterol)
- LDL (“Bad” Cholesterol) – High levels increase cardiovascular risk with supraphysiological dose of TRT, but physiological dose reduces LDL (28,)
- HDL (“Good” Cholesterol) – physiological TRT is now belived to have little impact on HDL, (29)
Liver Enzymes (ALT, AST)
- Oral AAS (e.g., Anavar, Dianabol) can stress the liver, but injectable or topical TRT has minimal impact
- We never use oral AAS in our research because of the impact on the liver
Blood Pressure (Ideal: ~120/80 mmHg)
- TRT can increase blood pressure, especially if hemoglobin/ hematocrit is high
- Monitor regularly to prevent hypertension-related issues
Insulin Sensitivity & Blood Sugar
- Measure fasting Blood Glucose & HbA1c (Long-term blood sugar control)
- TRT can improve insulin sensitivity, reducing risk of type 2 diabetes
The Benefits of AAS Use – Who Should Consider TRT or Other AAS? Optimization of Body and Health
Over the past 15 years, medical recommendations on exogenous testosterone have shifted dramatically. Initially, concerns about heart disease and other risks fueled caution, but newer evidence has overturned these fears.
Past Concerns vs. Updated Findings
- JAMA studies (2013, 2014) (7,8) reported a 30% increase in cardiovascular events in men with pre-existing heart disease.
- In 2014, the FDA warned about potential heart risks, partly due to overprescription in “low-T” clinics.
- However, by 2025, expert consensus supports TRT’s benefits, provided it’s used correctly and monitored by medical professionals.
When properly administered and supervised, the benefits of TRT and AAS far outweigh the risks.
Key Benefits of TRT & AAS in Medically Supervised Use
1. Physical Benefits
- Increased Muscle Mass & Strength – Boosts protein synthesis and nitrogen retention, leading to 3–5 kg of lean muscle gain per year.
- Fat Reduction – Enhances fat metabolism, particularly reducing visceral (abdominal) fat.
- Improved Bone Density – Prevents osteoporosis and strengthens spinal & hip bone mineral density (BMD).
- Enhanced Recovery & Performance – Increases red blood cell production, improving oxygen delivery and endurance.
2. Mental & Cognitive Benefits
- Higher Energy & Less Fatigue – Most men report feeling revitalized within weeks of starting TRT.
- Better Mood & Mental Health – Testosterone regulates dopamine and serotonin, reducing depression and anxiety.
- Cognitive Function – Some studies suggest testosterone improves memory and processing speed, potentially reducing the risk of Alzheimer’s disease.
3. Sexual & Reproductive Benefits
- Higher Libido & Improved Sexual Function – TRT boosts sex drive and erectile function in men with low T.
- Preserving Fertility (with hCG or SERMs) – While TRT alone reduces sperm count, combining it with hCG, GnRH, or SERMs (like Clomid) can maintain fertility.
4. Metabolic & Cardiovascular Benefits
- Improved Insulin Sensitivity – Lowers the risk of type 2 diabetes.
- Better Cholesterol & Heart Health – Can lower LDL (bad cholesterol) and increase HDL (good cholesterol).(28)
- Testosterone supports heart function when used responsibly, though excessive doses can increase CV risk.
Who Benefits Most from TRT?
Men experiencing clinically diagnosed low T (below ~400 ng/dL) with symptoms like:
- Androgen Deficiency in the Aging Male – The ADAM questionnaire
- Metabolic syndrome: elevated BP, obesity or insulin resistance
- Reduced muscle mass
- Lower energy, motivation or drive
- Reduced productivity
- Chronic fatigue
- Depression
- Decreased sex drive/low libido
- Poor sleep
- Erectile dysfunction
The informed medical community has reversed its stance on TRT, recognizing its overwhelming benefits when used responsibly. The fear surrounding AAS use stems largely from misuse, misinformation, and unsupervised administration. With proper medical oversight, AAS can be both safe and highly beneficial.
Health Blogs #2: Fasting – Another Healthcare Fad or a Real Health Benefit?
By Jonathan A. Jarman, MD
(~ 20 minute read without focus on the references)
(~ 22 min audio with references removed for an easier listen)
Introduction
Healthcare fads can explode like a wildfire in residential Los Angeles and garner just as much media attention. I think fasting falls into this category - tremendous hype, but some truth and benefit.
There’s some solid research that helps us separate the real benefits of fasting from the potential risks. But there’s also a lot of mediocre science that some treat like gospel, which only fuels the hype.
This isn’t surprising—nutrition research is often messy. Many nutrition studies rely on surveys, and most of us can’t accurately remember what we ate yesterday, let alone last week. In addition, those surveys can involve so many variables that it’s easy to mistake a simple association for true cause and effect, e.g. the Mediterranean Diet does such and such for our health. What is a Mediterranean Diet? There are many variables in the Mediterranean Diet, or any named diet for that matter, and to make a blanket conclusion that a multiple ingredient diet is the cause of x, y or z as regards our health is shoddy science. Shoddy science is common in nutrition research.
The task then is to identify quality research that may point us to potential benefits of fasting.
Fasting Blog Goals
In this Health Blog I will cut through the social media hype, address two types of fasting, the science behind the potential medical benefits and lastly how we might fast so that we can increase our chance of success.
There’s a lot of talk about fasting, so it helps to keep things simple. I like to think of fasting in two main ways: 1) Time-Restricted Eating (TRE), and 2) 24-hour fasting.
The biggest risk with fasting, whether TRE or 24 hour fasting, is muscle loss. Since building and keeping muscle is important for overall health, any fasting routine that causes muscle loss needs to offer big benefits to be worth it.
If someone drops a lot of body and visceral fat through regular fasting but loses just a little muscle, that could be a fair tradeoff. But with enough protein and resistance training between fasts, we can usually protect muscle—and even build more.
Let’s dive into the two types and the potential benefits of each.
- Time Restrictive Feeding (TRE)
TRE (Time-Restricted Eating) is an eating style that limits the daily period during which you consume calories to a specific, consistent window of time, while total caloric intake and other nutrients, specifically protein, is not reduced.
In TRE, one is consuming the SAME number of calories, but in a shorter eating window than one would if eating that number in a 24 hour period ad lib. If eating the same number of calories in a shorter window vs 24 hour ad lib has benefits such as weight loss, it proves that weight loss is not just due to eating fewer calories than one expends.
The theory of why benefits are seen in TRE are:
- Circadian rhythm alignment → optimal timing for metabolism.
- Fasting window → metabolic switch to fat/ketone use.
- Hormonal regulation → better appetite control.
- Glycemic control → improved insulin sensitivity.
- Cellular cleanup → autophagy, repair, and resilience.
I don’t want to spend much time on each of the above, but I do find the role of circadian timing in TRE interesting. The physiology of TRE is:
- Insulin sensitivity peaks earlier in the day
- In the morning to early afternoon, cells are more responsive to insulin, so glucose is cleared more efficiently.
- Later in the evening, insulin sensitivity drops, meaning the same food produces a bigger glucose and insulin spike.
- Digestive efficiency follows a daily cycle
- Enzymes and gut motility are higher earlier in the day, making nutrient processing smoother.
- Late eating slows digestion and may increase gut permeability and inflammation markers overnight.
- Nighttime eating conflicts with melatonin release
- Melatonin suppresses insulin secretion. Eating when melatonin is high (close to bedtime) can cause higher post-meal glucose levels.
- This is why late-night snacking is linked to impaired glucose tolerance even in healthy people.
- Circadian alignment supports downstream systems
- Liver glucose production, fat oxidation, blood pressure, and even mitochondrial function follow a day–night pattern.
- Eating “out of phase” (late) appears to disrupt these, independent of calorie intake.
For simplicity, I will use two common TRE (Time-Restricted Eating) windows as examples:
- 16:8 TRE
- Eat during an 8-hour window and fast for 16 hours.
- Example: Eating from 10:00 PM to 6:00 PM (8 hours), fasting from 6:00 PM to 10:00 PM (16 hours) the next day.
- 14:10 TRE
- Eat during a 10-hour window and fast for 14 hours.
- Example: eating from 8:00 AM to 6:00 PM (10 hours), fasting from 6:00 PM to 8:00 AM the next day (14 hours).
With each of these I set a cutoff of 6pm to avoid eating close to bedtime.
You might then ask whether the benefits of TRE come from avoiding eating late or close to bedtime. That’s a great question, and I’ll address it later in this Blog
Since we have now defined two TRE options, what are the researched based potential benefits of TRE vs unrestrictive eating periods?
There are 6 potential benefits with excellent research by Gabel, Sutton, Wilkinson Moro and Jamshed.
- Reduced Body Fat & Improved Body Composition
TRE (like an 8-hour eating window) helps reduce fat mass even without cutting calories, promoting a healthier body composition
(Gabel, K., et al. (2018). Effects of 8-hour time restricted feeding on body weight and metabolic disease risk factors in obese adults: A pilot study. Nutrition and Healthy Aging, 4(4), 345–353.
- Improved Insulin Sensitivity & Glucose Regulation
Eating within an earlier, restricted window boosts insulin sensitivity and controls blood sugar better—even without weight loss
(Sutton, E. F., et al. (2018). Early Time-Restricted Feeding Improves Insulin Sensitivity, Blood Pressure, and Oxidative Stress Even Without Weight Loss in Men with Prediabetes. Cell Metabolism, 27(6), 1212-1221.e3.
- Better Cardiometabolic Health
TRE lowers blood pressure, bad cholesterol (LDL), and triglycerides, improving heart health markers
(Wilkinson, M. J., et al. (2020). Ten-Hour Time-Restricted Eating Reduces Weight, Blood Pressure, and Atherogenic Lipids in Patients with Metabolic Syndrome. Cell Metabolism, 31(1
- Improved Circadian Rhythm Alignment
Aligning eating with natural circadian rhythms optimizes metabolism and hormone function, enhancing overall metabolic health
(Panda, S. (2016). Circadian physiology of metabolism. Science, 354(6315), 1008-1015.
- Reduced Appetite & Improved Satiety Signals
TRE normalizes hunger hormones, which helps control appetite and may lead to reduced calorie intake naturally
(Hutchison, A. T., et al. (2019). Effects of intermittent fasting on appetite: A randomized controlled trial. Nutrients, 11(2), 320
- Cellular & Molecular Benefits
Fasting periods during TRE activates cellular repair processes like autophagy, which reduces oxidative stress and supports healthy aging.
Autophagy is like your body’s housekeeping service—taking out the trashy, worn-out cells so the fresh ones can do their job without the clutter.
(Longo, V. D., & Panda, S. (2016). Fasting, Circadian Rhythms, and Time-Restricted Feeding in Healthy Lifespan. Cell Metabolism, 23(6), 1048-1059.).
What about TRE biomarker benefits?
There are 8 known biomarker benefits of TRE and again we see some of the better research studies by the aforementioned authors.
- Fasting Insulin & Insulin Sensitivity
- Improvement: TRE significantly lowered fasting insulin levels, meaning the pancreas released less insulin to control blood sugar.
- How: The body became more insulin sensitive, so cells responded better to insulin, enabling more efficient glucose uptake and reduced insulin demand (Sutton et al., 2018).
- Fasting Glucose & HbA1c
- Improvement: TRE reduced or stabilized fasting blood glucose and caused modest decreases in HbA1c.
- How: Better insulin sensitivity and improved glucose metabolism resulted in more stable blood sugar levels over time, reducing the average blood glucose exposure reflected by HbA1c (Gabel et al., 2018; Wilkinson et al., 2020).
- Lipid Profile (LDL, Triglycerides, HDL)
- Improvement: TRE lowered LDL cholesterol and triglycerides, while maintaining or slightly increasing HDL.
- How: Extended fasting periods enhance fat metabolism, promoting breakdown of stored fat and improving lipid clearance from the bloodstream, thus reducing atherogenic lipids (Wilkinson et al., 2020; Antoni et al., 2018).
- Blood Pressure
- Improvement: Both systolic and diastolic blood pressure decreased modestly.
- How: Improved insulin sensitivity and lower oxidative stress reduce vascular inflammation and stiffness, which helps blood vessels relax and lowers blood pressure (Sutton et al., 2018; Antoni et al., 2018).
- Inflammatory Markers (CRP)
- Improvement: TRE reduced circulating C-reactive protein (CRP), indicating decreased systemic inflammation.
- How: Fasting reduces pro-inflammatory cytokines and oxidative stress, calming chronic low-grade inflammation (Antoni et al., 2017).
- Appetite-Regulating Hormones (Leptin, Ghrelin)
- Improvement: TRE normalized leptin and ghrelin levels, improving hunger and fullness cues.
- How: Leptin sensitivity improved, helping signal satiety effectively, while ghrelin fluctuations were better controlled, reducing excessive hunger and cravings (Moro et al., 2016).
- Oxidative Stress Markers
- Improvement: Markers of oxidative stress, such as F2-isoprostanes, decreased.
- How: Fasting boosts antioxidant defenses and reduces reactive oxygen species production, lowering cellular damage (Sutton et al., 2018; Moro et al., 2016).
- Circadian Hormones (Cortisol, Melatonin)
- Improvement: TRE helped normalize the daily rhythms of cortisol and melatonin.
- How: Aligning eating times with natural light-dark cycles supports the body’s internal clock, improving hormone regulation, metabolism, and sleep quality (Gill & Panda, 2015).
But why does TRE improve fat loss and metabolism when calories are the same as in unrestricted eating?
Based on current science and some of the theory touched on earlier:
- Circadian Rhythm Alignment
Our metabolism follows a daily rhythm controlled by our internal biological clock. TRE helps align food intake with this rhythm:
- During the day, your body is primed to digest and metabolize food efficiently.
- At night, metabolism slows, insulin sensitivity decreases, and the body favors fat storage.
Eating late or across a long window disrupts this natural timing, promoting fat accumulation and metabolic dysfunction.
- Extended Fasting Benefits
The fasting period between eating windows triggers beneficial metabolic switches:
- After about 12 hours of fasting, the body shifts from using glucose to burning stored fat (fat oxidation).
- Fasting promotes hormone changes (lower insulin, higher growth hormone) that favor fat breakdown.
- Cellular repair processes like autophagy kick in, improving metabolic health.
- Reduced Insulin Exposure and Improved Insulin Sensitivity
By limiting the eating window, you reduce the total time your body spends processing food and insulin production. This can improve insulin sensitivity and reduce fat storage signals, even if calorie intake is unchanged.
- Improved Mitochondrial and Metabolic Efficiency
Time-restricted feeding may improve mitochondrial function and how efficiently your cells use energy, reducing oxidative stress and improving fat metabolism.
There is a big question media and hype machines fail to ask. Might a big part of TRE’s benefits come from avoiding eating late at night or close to bedtime, rather than just from the total length of the fasting window itself?
Indeed, the timing of eating, especially avoiding food intake close to bedtime, may be a key driver of TRE’s benefits — not just the fasting period length itself.
As you may have noted earlier in this Blog, some research suggests that a big part of TRE’s benefits might come from avoiding eating late at night or close to bedtime, rather than just from the total length of the fasting window itself. Some research, however, shows that even more restrictive TRE has greater metabolic benefit suggesting the benefit is not due to eating cessation well before bedtime.
- Sutton, E. F., et al. (2018).
Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes.
- This study showed improved insulin sensitivity and blood pressure when eating was limited to 8 am–2 pm versus typical eating patterns, highlighting benefits of early TRE.
Cell Metabolism, 27(6), 1212-1221.e3.
- Jamshed, H., et al. (2019).
Early time-restricted feeding improves 24-hour glucose levels and affects markers of the circadian clock, aging, and autophagy in humans. - Demonstrated improved glucose regulation and circadian rhythm markers with early TRE (6 am–3 pm).
Nutrients, 11(6), 1234.
5.Nighttime eating is linked to increased risk of obesity and metabolic disease independent of calories:
- This review links late-night eating and circadian misalignment to increased obesity and diabetes risk, beyond total caloric intake.
McHill, A. W., & Wright, K. P. Jr. (2017).Role of sleep and circadian disruption on energy balance and diabetes: A summary of workshop discussions.
Clinical Therapeutics, 39(5), 930-937. - Meta-analysis showing night eating is associated with higher obesity risk independent of calorie consumption. Zhu, L., et al. (2019). Night eating and risk of obesity: A systematic review and meta-analysis.
International Journal of Obesity, 43(6), 1210-1217.
The takeaway:
Even with the same calories, the research shows that when you eat affects your hormones, metabolism, and how your body partitions energy. TRE “resets” or optimizes these daily rhythms, making your metabolism work better — burning more fat and improving health — compared to eating the same calories scattered over a longer time or late at night.
- 24 Hour Fasting
This is where I have greater regarding muscle loss and so we must ask are there any potential additional benefits to periodic 24 hour fasting over TRE? Might the two fasting protocols be done in conjunction?
The commonly recommended and researched frequencies are: 1–2, 24-hour fasts weekly or 24 hours fasts every 2 -4 weeks.
Why might 24 hour fasting provide additional benefits to TRE?
There are 6 suggested additional benefits for 24 hour fasting over TRE:
- Deeper Ketosis & Fat Burning
Describes ketone production increase during prolonged fasting beyond shorter fasts.
(Cahill, G. F. Jr. (2006). Fuel metabolism in starvation. Annual Review of Nutrition, 26, 1-22.)
- Stronger Activation of Autophagy and Cellular Repair
Highlights autophagy induction with longer fasting durations.
(Mizushima, N., & Komatsu, M. (2011). Autophagy: renovation of cells and tissues. Cell, 147(4), 728-741.)
(Longo, V. D., & Mattson, M. P. (2014). Fasting: Molecular mechanisms and clinical applications. Cell Metabolism, 19(2), 181-192.)
- Greater Reduction in Insulin and Blood Glucose
(Halberg, N., et al. (2005). Effect of intermittent fasting and refeeding on insulin action in healthy men. Journal of Applied Physiology, 99(6), 2128-2136.)
- Significant Growth Hormone Surge
(Ho, K. Y., et al. (1988). Fasting enhances growth hormone secretion and amplifies the complex rhythms of growth hormone secretion in man. The Journal of Clinical Investigation, 81(4), 968-975.)
- More Pronounced Anti-Inflammatory Effects
(Antoni, R., et al. (2017). Effects of intermittent fasting on markers of inflammation: A systematic review and meta-analysis. Clinical Nutrition, 36(3), 795-806.)
- Potential Enhanced Cognitive and Neuroprotective Effects
(Mattson, M. P., et al. (2018). Intermittent metabolic switching, neuroplasticity and brain health. Nature Reviews Neuroscience, 19(2), 63-80.
What about biomarker proof of 24 hour fasting benefits?
It is important that we have a way to measure the potential benefits of periodic 24 hour fasting over TRE. The following biomarker benefit are unique to, or more pronounced, in periodic 24-hour fasting based on controlled human trials as compared to typical TRE:
Fasting Insulin → Decreases, indicating improved insulin sensitivity
- Harvie, M. N., et al. (2011). The effects of intermittent or continuous energy restriction on weight loss and metabolic disease risk markers: a randomized trial in young overweight women.International Journal of Obesity, 35(5), 714–727. https://doi.org/10.1038/ijo.2010.171
Fasting Glucose → Often modestly reduced or stabilized
- Trepanowski, J. F., et al. (2017). Effect of alternate-day fasting on weight loss, weight maintenance, and cardio protection among metabolically healthy obese adults: a randomized clinical trial.JAMA Internal Medicine, 177(7), 930–938. https://doi.org/10.1001/jamainternmed.2017.0936
HbA1c → Can decrease over weeks–months if elevated at baseline
- Carter, S., et al. (2018). Effect of intermittent compared with continuous energy restriction on glycemic control in patients with type 2 diabetes: a randomized noninferiority trial.JAMA Network Open, 1(3), e180756. https://doi.org/10.1001/jamanetworkopen.2018.0756
LDL Cholesterol → Tends to decrease
- Trepanowski, J. F., et al. (2017). (same as above)
Triglycerides → Often significantly reduced
- Varady, K. A., et al. (2009). Short-term modified alternate-day fasting: a novel dietary strategy for weight loss and cardio protection in obese adults.American Journal of Clinical Nutrition, 90(5), 1138–1143. https://doi.org/10.3945/ajcn.2009.28380
HDL Cholesterol → Typically stable or slightly increased
- Varady, K. A., et al. (2009). (same as above)
Blood Pressure → Modest reduction in systolic and diastolic values
- Harvie, M. N., et al. (2011). (same as above)
C-reactive Protein (CRP) → Decreases, reflecting reduced systemic inflammation
- Kroeger, C. M., et al. (2012). Impact of weight loss by alternate day fasting on markers of chronic disease risk in obese adults.Obesity, 20(9), 1836–1841. https://doi.org/10.1038/oby.2012.63
Ketone Levels → Increase markedly during the fast, reflecting metabolic shift to fat-burning
- Halberg, N., et al. (2005). Effect of intermittent fasting and refeeding on insulin action in healthy men.Journal of Applied Physiology, 99(6), 2128–2136. https://doi.org/10.1152/japplphysiol.00683.2005
Oxidative Stress Markers (e.g., F2-isoprostanes) → Reduced
- Johnson, J. B., et al. (2007). Alternate day calorie restriction improves clinical findings and reduces markers of oxidative stress and inflammation in overweight adults with moderate asthma.Free Radical Biology and Medicine, 42(5), 665–674. https://doi.org/10.1016/j.freeradbiomed.2006.12.005
IGF-1 → Often decreases, potentially lowering growth signaling linked to aging and cancer risk
- Fontana, L., et al. (2008). Long-term calorie restriction is highly effective in reducing circulating IGF-1 and its bioavailable fraction in humans.Aging Cell, 7(5), 681–687. https://doi.org/10.1111/j.1474-9726.2008.00417.x
I will argue that the ONLY way we would know if these biomarker benefits occurred just from 24 fasting is if we keep our body composition the same at the end of some defined period. This is part of the problem with this type of research – too many variables. Did we get better biomarkers because of calorie restriction from these 24 hour fasts and body fat loss of just from the fast? I don’t think we know the answer to this.
- How to Fast: 13 Strategies That Help
If this information motivates you to try one or both of the defined types of fasting in this blog, I recommend the following:
24 hour fasts:
- If you’re younger, well-trained, and eating adequate protein + strength training, 1–2 weekly 24-hour fasts might be fine.
- If you’re older, less trained, or worried about muscle loss, spacing fasts every 2 weeks or monthly may be safer and more sustainable.
It is imperative to monitor your body composition, strength, and recovery to adjust frequency using Dexascan for body composition and Heart Rate Variability (HRV) monitors for recovery.
HRV can help track how well you recover from fasting stress. Rising or stable HRV during fasting cycles is a good sign. Declining HRV may signal over-stress, prompting modifications.
If you choose to follow these fasting protocols, these 13 tips can make both TRE and 24 hour fasting easier.
- Start Slow
- Begin with shorter fasting windows (like 12-14 hours) before moving to longer fasts. Gradually increase as your body adapts.
- Stay Hydrated
- Sometimes thirst is mistaken for hunger. Drink plenty of fluid throughout the fasting period. Electrolyte water, herbal teas, green tea, black coffee, or sparkling water can help curb hunger without breaking the fast. Caffeine in many of these drinks help curb appetite. Make sure all are without added sugars.
- Keep Busy
- Distraction helps — keep yourself occupied with work, hobbies, or light activities to take your mind off hunger. Avoid, or at least limit, TV after the last meal in TRE.
- Focus on Quality Meals When Eating
- Eat nutrient-dense, balanced meals rich in protein, fiber, healthy fats alongside complex carbs can help you feel fuller longer and make fasting easier. This keeps you full longer and supports muscle retention. So, avoid sugars a simple carbs as they make you hungrier sooner.
- Adjust Exercise Timing
- Do resistance training or more intense workouts during your eating window or shortly after to optimize muscle maintenance and recovery.
- Listen to Your Body
- If you feel dizzy, weak, or overly fatigued, it’s okay to break the fast or adjust the fasting length. Safety first.
- Set a Consistent Schedule
- Try to fast and eat around the same times daily to train your body’s internal clock and reduce hunger fluctuations.
- Limit Exposure to Food Triggers
- Avoid environments or situations that tempt you to eat outside your window, like browsing social media food posts or frequent snacking areas.
- Get Good Sleep
- Poor sleep increases hunger hormones and cravings. Prioritize sleep hygiene to support fasting success.
- Fiber
- There are two forms of commercial fiber – capsules and powder. Use either form every few hours to help feel full during the 24 hour fast and with the last meal during TRE.
- With TRE fasting
- Continue to eat 1 gm/protein/24 hours/ideal body weight during the eating period.
- Make your last TRE meal high in both protein and fiber to keep satiety longer.
- Use a casein supplement with your last meal because casein digests slowly and will help maintain satiety.
- Television
- It is advisable to avoid or limit watching television after your last meal within the TRE window, as commercials often promote snacking, which may undermine your fasting objectives. And yes this has been repeated intentionally. The enemy is that large bowl of ice cream or cake while watching TV.
- Engage in Light Physical Activity
- Gentle exercise, such as walking or stretching, can help distract from hunger and improve mood without overly stressing the body.
Summary
There is science to support both fasting strategies as valuable tools for improving metabolic health and reducing chronic disease risk when tailored to the right person and implemented mindfully so that muscle loss does not occur. However, many variables are in flux. As I previously said, with either TRE or 24 hour fasts, is the fast the benefit or if a change in body composition what is occurring? Whichever it is, there appears to be physiologic biomarker benefit.
Individual factors such as age, activity level, muscle mass, and overall health determine optimal fasting frequency and approach.
Combining fasting with adequate protein intake and resistance training maximizes benefits and minimizes risks.
And decide what fasting protocols can you live with.
__________________
I hope you enjoyed this Tip and benefit from it.
If you have any questions or comments, please don’t hesitate to share them!
Health Blogs #3: Functional Medicine, Wellness Culture, and the Rise of Fringe Medicine: An Evidence-Based Evaluation
By Jonathan A. Jarman, MD
We are often asked whether the Foundation is based on so-called “Functional Medicine” or “Wellness Medicine.” It is not.
In fact, some of the most common questions we receive—from friends, donors, and research participants—arise from Functional Medicine and Wellness posts circulating on social media. These posts frequently demonize well-established, scientifically supported medical treatments, using fear based rhetoric such as “your doctor doesn’t want you to know this” or “Big Pharma is hiding the cure.” Immediately afterward, they promote unproven supplements, detox kits, anti-aging elixirs, hormonal “balancers,” or specialized lab tests with little to no qualified research supporting their use.¹ ² ³
A high-profile example of this phenomenon is Dr. Mehmet Oz, formerly featured on the Oprah network and host of The Dr. Oz Show. Over the years, he promoted dietary supplements such as green coffee bean extract, garcinia cambogia, and raspberry ketones, often calling them “miracle” products despite limited or conflicting evidence. He also made controversial claims about treatments such as hydroxychloroquine for COVID-19, which were not supported by rigorous scientific consensus. Critics highlighted that many of his recommendations were not evidence-based, illustrating how celebrity authority amplifies commercial wellness messaging and misleads the public.¹¹ ¹²
There is no evidence Dr. Oz personally profited from the supplement companies he highlighted; however, his endorsements produced enormous commercial gains for those companies and significantly increased his show’s viewership, creating powerful indirect incentives.¹³ ¹⁴ ¹⁵ ¹⁶
The Federal Trade Commission (FTC) found that companies using Dr. Oz’s appearance (or referencing it) still made millions via the “Oz effect” when they promoted green coffee bean extract and related supplements — e.g., t*he company agreed to a settlement and prohibition of misleading claims.* ¹⁵
Oz himself stated that after airing a segment promoting green coffee bean extract, “the Internet lit up … ads proliferated … the result is the same — my viewers are still victims of fraud and false claims by a sophisticated … enterprise.” (from his testimony) ¹⁴
Many social media health ads rely on fear-based messaging, using phrases like “don’t wait until it’s too late”, “Big Pharma hates this natural secret,” “What your lab work really means (your doctor probably never checked this),’ “This simple at-home test reveals hidden imbalances doctors overlook,” “You don’t have to feel this way — most doctors won’t tell you this.” psychological tactics shown to increase consumer urgency and reduce critical thinking.
Fear-based messages are not accidental; they are high-conversion marketing strategies that reliably drive supplement sales, affiliate revenue, and program enrollment by keeping the audience in a constant state of perceived biological vulnerability.
Fear is also central to the modern snake-oil playbook: the marketer manufactures anxiety about unseen dangers and then presents a supplement, detox, or genetic panel as the only lifeline available — a technique as old as medicine shows, now repackaged for Instagram and TikTok.
The challenge for the Foundation lies in explaining why these fear based “fountain of youth” products cannot do what they claim. Many are marketed with scientific-sounding language*—detoxification pathways, inflammation markers, SNP variants, mitochondrial boosters—but almost none are grounded in *validated human research or clinical outcomes.² ³ ⁵ Our experience has been consistent: the vast majority—*easily 99%—of social media posts selling a supplement, genetic panel, or bespoke lab test for “optimal health” are promoting products that deliver *no meaningful clinical benefit. They are modern versions of snake oil, seemingly crafted under the marketing philosophy that PT Barnum was right when he said, “There’s a sucker born every minute.” These posts exploit natural human hope for health, youth, and control while enriching the influencer, clinician, or supplement distributor—whether an MD or an unlicensed wellness promoter—far more than they help the patient.² ⁷
The Foundation’s mission is the opposite. We aim to advance traditional Western medicine by preserving its rigorous standard for diagnosis and treatment while adding a complementary focus on health optimization, quality of life, and longevity. Our goal is to explore what true optimization looks like using rigorous scientific methods, not commercialized shortcuts or pseudoscientific claims repackaged as **“root-cause solutions.”**⁸
What Functional Medicine Says It Is
Functional Medicine describes itself as a patient-centered, systems-oriented model that seeks to understand the “root causes” of disease rather than treating symptoms. It emphasizes:
- Extensive personal histories
- Nutrition, lifestyle, and environmental factors
- Long-format visits
- A partnership model between clinician and patient¹
In principle, we agree that this sounds attractive and addresses real shortcomings in conventional Western medical care. But in practice, Functional Medicine often blends legitimate holistic concepts with unvalidated testing, speculative biology, premature clinical claims, and commercial supplement protocols—placing large portions of the field within fringe medicine.⁴ ⁷
Why Patients Gravitate Toward Functional Medicine
The appeal is understandable. Conventional Western medicine, constrained by brief clinic visits, heavy documentation burdens, and insurance-driven limitations, often struggles to provide the time and comprehensive lifestyle guidance patients want. Functional Medicine practitioners typically:
- Do not accept insurance – and this is fine
- Spend more time with patients
- Integrate behavioral and lifestyle discussions
- Offer whole-person explanations
- Provide structure, validation, and a coherent narrative
These attributes are indeed meaningful. They foster psychological and relational healing, which conventional Western medicine sometimes neglects.
Holistic engagement is not the issue. The issue is how Functional Medicine interprets and intervenes on those narratives.
Where Functional Medicine Shows Real Strength
Functional Medicine gets several things right—things traditional medicine should embrace more explicitly:
- Lifestyle matters profoundly
- Behavior change requires time and trust
- Stress, sleep, and diet shape chronic disease² ³
- Patients benefit from systems-level thinking
- The biopsychosocial model is indispensable⁶ ⁸
These strengths are not proprietary to Functional Medicine, but the field often frames them as if they were. Evidence-based medicine should reclaim these concepts without importing the unsupported methods that frequently accompany them.
Where Functional Medicine Becomes Fringe Medicine
Despite admirable intentions, Functional Medicine suffers from serious scientific, methodological, and ethical weaknesses.
1. Reliance on Non-Validated Testing
Functional Medicine commonly uses tests not recognized as diagnostic by major medical societies, including:
- IgG food sensitivity panels
- Cortisol rhythm saliva tests
- Microbiome stool assays lacking clinical endpoints
- Heavy metal “challenge tests”
- Broad hormone panels in otherwise healthy individuals
- Toxin panels with undefined thresholds¹ ⁴ ⁷
These tests often produce abnormal results because they’re designed to, providing justification for costly supplement regimens and reinforcing the snake-oil cycle.² ⁴
2. Mechanistic Reasoning Treated as Clinical Evidence
Functional Medicine often extrapolates from basic physiology (e.g., gut permeability, methylation pathways) and treats these mechanisms as proven clinical drivers of symptoms. This leap—from mechanism to medicine—is where science frequently breaks.⁵
3. Supplement-Based Treatment Models
Functional Medicine practitioners often recommend:
- High-dose vitamins
- Proprietary blends
- Detox powders
- Hormone-optimizing supplements
- Specialized mitochondrial/anti-aging products² ⁴
Many clinics sell these supplements directly, creating clear conflicts of interest and reinforcing the *commercial nature*of the interventions.²
4. Lack of Standardization
Two practitioners may interpret the same labs in completely different ways or recommend wildly different protocols. This variability reflects ideology, not evidence.⁴ ⁷
5. Absence of Robust Clinical Research
The interventions most unique to Functional Medicine—*detox packages*, SNP-driven supplement plans, organ “support” regimens—lack controlled clinical trials demonstrating efficacy.⁴ ⁹ ¹⁰
These weaknesses collectively push Functional Medicine into fringe medicine territory.
The Misuse of Genetic and DNA Testing
A particularly concerning trend is the industry’s use of DNA testing to create personalized supplement prescriptions. Many clinics market SNP-based testing—such as *MTHFR, COMT, APOE, VDR*—as a roadmap for:
- Micronutrient dosing
- Methylation support
- Detox pathway optimization
- Neurotransmitter modulation
- Anti-aging regimens
However:
- Most SNPs have *minuscule effect sizes*⁹ ¹⁰
- They are not predictive of disease in healthy individuals⁹
- No major society endorses *SNP-guided therapy*⁸ ⁹
- Genetic tests often create *false risk perceptions*⁹
- Supplement plans based on SNPs lack *clinical validation*⁹ ¹⁰
What appears to be precision medicine is often scientific storytelling.
Where Functional Medicine and Wellness Culture Intersect
Functional Medicine blends seamlessly into the modern Wellness industry, which mixes legitimate lifestyle science with commercial pseudoscience.² ³ ⁶
-
Health as a purchasable commodity
-
Fear-based marketing
-
Illusion of control
-
Overmedicalization of normal life
-
Exploiting vague symptoms
Another powerful marketing tactic is the appeal to “natural” products. Wellness advertising frequently implies that “natural” substances are inherently safer, gentler, or more effective than conventional treatments. This is scientifically meaningless. *Nature produces some of the most toxic compounds known to medicine*—botulinum toxin, cyanide, ricin, and belladonna are all “natural.” Conversely, many of the safest and most life-saving treatments in modern medicine are highly refined or fully synthetic. The “natural equals safe” narrative persists because it feels intuitive and comforting, not because it reflects toxicology or clinical data. It is a marketing illusion, one that allows supplement companies to bypass the regulatory scrutiny required of pharmaceuticals while cultivating consumer trust through a scientifically empty label claim.
Marketers contrast frightening portrayals of pharmaceuticals with soothing claims of “natural” alternatives, creating a fear-versus-comfort dichotomy that has no grounding in pharmacology or toxicology, but is highly effective at selling products.
6. Manipulative Social Media Tactics
Functional Medicine influencers and wellness marketers frequently use:
• Demonization of evidence-based medicine² ³
• Partial truths blended with falsehoods³
• Emotionally charged fear statements
• Anecdotes as evidence
• Claims of secret knowledge
• *Direct product links*²
These tactics prime patients to distrust validated care and purchase unregulated supplements, continuing the snake-oil cycle.² ⁷
Practitioner Qualifications and Lack of Board Certification
Functional Medicine practitioners come from widely variable backgrounds. Crucially:
• Functional Medicine is not recognized by the American Board of Medical Specialties.¹
• There is no accredited board certification in Functional Medicine.¹
• Training programs vary widely in rigor and scientific oversight.⁴
This makes it difficult for patients to distinguish between evidence-informed care and fringe practice.
Integrating the Best of Both Worlds—Without the Pseudoscience
The future of medicine lies in combining relational, behavioral, and systems-oriented care with methodological rigor*and *validated interventions.⁶ ⁸
Patients deserve both:
• holism, and
• evidence.
Conclusion
Functional Medicine arose to address real gaps in healthcare. However, its reliance on unvalidated tests, supplement-driven revenue, genetic overinterpretation, and social-media-driven pseudoscience places large portions of the field within fringe medicine.² ³ ⁴ ⁷ ⁹ ¹⁰
Holism without rigor is not progress.
Science without empathy is not healing.
Patients deserve both.
And that is the gap the Foundation seeks to bridge—using rigorous scientific research, not *commercial pseudoscience*disguised as health optimization.⁸
Please let us know if you have and questions or comments. We greatly appreciate your feedback.
References
-
Institute for Functional Medicine (IFM). What is Functional Medicine? 2024.
-
Cohen PA et al. “The Supplement Industry and Conflicts of Interest.” JAMA, 2024.
-
Turner L. “Commercial Wellness, Pseudoscience, and Consumer Risk.” Health Policy, 2023.
-
American Council on Science and Health (ACSH). “Evaluating Functional Medicine Claims.” 2025.
-
Ioannidis JPA. “Why Most Mechanistic Explanations Fail.” eLife, 2023.
-
Caulfield T. Wellness Culture and the Meaning of Health. Oxford University Press, 2024.
-
Barrett S. “Dubious Treatments and Fringe Medical Practices.” Quackwatch, 2024.
-
National Academies of Sciences. Integrative Health and Evidence Standards, 2023.
-
Green RC et al. “Clinical Utility of Genetic Testing.” New England Journal of Medicine, 2024.
-
Burke W et al. “Interpreting SNP-Based Genomic Information.” Genetics in Medicine, 2023.
-
Inquirer.com. “Oz Promoted Pseudoscientific Supplements.” 2022.
-
WashingtonPost.com. “Dr. Oz and the Ethics of Celebrity Medicine.” 2022.
-
Tilburt JC, Allyse M, Hafferty FW. The Case of Dr. Oz: Ethics, Evidence, and Does Professional Self-Regulation Work? AMA Journal of Ethics. 2017;19(2):199–206.
14. U.S. Senate Committee on Commerce, Science, and Transportation. Hearing: Protecting Consumers from False and Deceptive Advertising of Weight-Loss Products. 113th Cong., June 17, 2014.
15. Federal Trade Commission. Marketer Who Promoted a Green Coffee Bean Weight-Loss Supplement Agrees to Settle FTC Charges. January 26, 2015.
16. Belluz J. “Government confirms one of Dr. Oz’s favored diet pills is a total hoax.” Vox. January 26, 2015.
Health Blog #5 The Quiet Brain: Why Emotional Control Determines High-Level Sports Performance — and the Medications That Can Help
By Jonathan A. Jarman, MD
It has always amazed me that athletes like John McEnroe or Jimmy Connors could lose control of their emotions and still compete at an extraordinarily high level. They remain rare exceptions. And it raises an important question: might they have achieved even greater success had they been able to regulate their emotions more consistently? They reached the pinnacle, of course—but even they might have benefited from greater emotional stability.
For most athletes—whether in tennis, golf, baseball, archery, track, cycling, or basketball—elite performance emerges from a quiet, disciplined mind rather than an emotionally charged one.
In my own experience as an amateur athlete—one who, like many kids, fantasized about someday becoming a professional—I learned early what it felt like to be both dialed in and completely thrown off. There were moments when I was fully locked onto the task, such as timing a baseball perfectly off the bat at age 12. And then there were other moments—like when a sharply bouncing ball came toward me at second base—when I felt a sudden surge of anxiety interrupt that clarity.
The contrast was unmistakable: one state felt effortless, the other constricting. I eventually moved to catcher to confront and control that instinctive spike of fear.
That early awareness of how emotion can hijack performance is part of what later drove my interest in the neuroscience behind the quiet mind.
This blog is about fine-tuning the brain for high-level performance—quieting the internal noise of the emotional system so the athlete can fully engage in the task at hand with maximal precision, timing, and execution. This approach reflects the Foundation’s broader mission: advancing true health and performance optimization rather than limiting care to disease management, as is common in Western medicine.
As an MD with a background in biochemistry and psychiatry, I will focus on the biology, physiology, and pharmacology of emotional control—less on the psychology—because the quiet brain is fundamentally a neurobiological state.
If you’re interested in the psychological side, the classic 1970s book Inner Tennis by W. Timothy Gallwey is foundational. Decades before neuroscience validated his ideas, Gallwey described how internal chatter disrupts skilled performance and how awareness, trust, and non-judgmental attention unlock fluid, high-level execution. Despite its title, the book is not about tennis—it is a universal manual for the mental side of all sports.
Across nearly every sport, the athletes who excel under pressure share a hidden advantage: they minimize internal noise. It’s why a 40-year-old Tom Brady can orchestrate a flawless two-minute drill, or why Novak Djokovic can face triple break point in a fifth set and hit with the same smooth precision he had in the first. Their movements don’t tighten. Their vision doesn’t constrict. Their decision-making doesn’t collapse.
Most observers call this mental toughness.
Neuroscience calls it limbic quiet.
The Neuroscience of a Quiet Brain
High-level sports performance, whether at the professional or amateur level, depends on keeping the prefrontal cortex (PFC)—the brain’s strategic and high-precision decision center—fully online¹,². At the same time, the limbic system—the emotional circuitry that generates frustration, fear, anger, and anxiety—must remain quiet³.
Even subtle limbic activation can:
- narrow visual fields⁴
- disrupt motor timing⁵
- increase muscle tension⁶
- degrade reaction time⁷
Athletes recognize this intuitively:
- When the limbic system intrudes, the game feels tight, rushed, chaotic.
- When it stays quiet, performance becomes smooth, efficient, and seemingly effortless.
This optimal mode is known as the flow state—a condition in which the brain is simultaneously calm and highly focused⁸. In flow:
- the PFC operates with maximal efficiency
- the limbic system goes nearly silent⁹
- the cerebellum automatically sequences movement¹⁰
- time perception changes, often slowing subjectively¹¹
Flow is not intensity.
Flow is the absence of internal noise¹².
Some athletes are naturally wired for limbic quiet. Many are not. Genetics, temperament, early conditioning, ADHD traits, anxiety tendencies, trauma exposure, and chronic stress all influence how easily the emotional brain hijacks performance¹³.
This explains why an athlete can dominate on Tuesday yet unravel on Thursday: the physiology is unchanged, but the internal noise level is not.
The Autonomic Nervous System: The Hidden Driver of Emotional Quiet
One crucial component of emotional quiet is often underestimated: the autonomic nervous system (ANS). The quiet brain is not simply a matter of prefrontal control over limbic emotion; it is also a dynamic interplay between the sympathetic (“fight or flight”) and parasympathetic (“rest and focus”) branches of the ANS.
When the sympathetic system surges—from frustration, anger, fear, or pressure—it immediately:
- tightens muscle tone
- increases tremor
- narrows visual attention
- destabilizes motor timing
- amplifies limbic reactivity
These shifts can occur in under 150 milliseconds and disrupt the fine-motor precision needed in tennis, golf, baseball, basketball, and nearly every other sport.
In contrast, parasympathetic activation provides the physiological foundation for:
- relaxed musculature
- steady breathing
- wide perceptual fields
- stable heart rhythms
- optimal PFC function
Parasympathetic tone is the bodily counterpart to the quiet mind.
This is why athletes rely on:
- controlled breathing
- pre-shot routines
- posture resets
- between-point rituals
These methods shift the ANS away from sympathetic dominance and toward the calm, stabilized state that supports clarity, precision, and flow.
Importantly, many of the medical interventions discussed later work, in part, by modulating the ANS—either blunting sympathetic surges or increasing parasympathetic stability.
HRV: The Biomarker of Internal Noise
Heart Rate Variability (HRV) is one of the most powerful physiological markers of emotional quiet and neural readiness. HRV reflects the balance between sympathetic and parasympathetic activity and correlates strongly with cognitive performance and emotional regulation¹⁴,¹⁵.
- High HRV = calm physiology, wide perception, smooth motor control, strong PFC performance
- Low HRV = sympathetic dominance, emotional noise, visual narrowing, impaired timing
HRV offers a numerical fingerprint of an athlete’s internal state.
Research consistently shows that higher HRV is associated with better executive function, improved reaction time, greater emotional resilience, and easier entry into flow¹⁶,¹⁷.
Many of the interventions in this blog—including propranolol, clonidine, guanfacine, controlled breathing, and structured routines—work partly by stabilizing HRV, making the quiet brain more accessible under pressure.
There are many HRV tracking systems available; I personally recommend the Morpheus Training System for its accuracy and practicality.
Why Quiet Minds Win
Sports require rapid integration of:
- motor planning
- spatial perception
- prediction
- decision-making
These processes rely on coordinated activity across the dorsolateral PFC, premotor cortex, cerebellum, and parietal visual-spatial networks¹⁸,¹⁹.
When these systems operate smoothly:
- movements feel fluid
- vision is broad
- timing feels natural
- decisions appear instantaneous
When the limbic system activates:
- heart rate surges²⁰
- tremor increases²¹
- attention narrows²²
- muscles stiffen²³
- prediction errors increase²⁴
And these changes occur faster than conscious control.
Some athletes maintain emotional quiet through personal techniques—e.g., Rafael Nadal’s ritualized routines, Simone Biles’ dissociation-coded breathing, or Steph Curry’s smile-reset posture—but when neurobiology overwhelms psychological strategies, medical interventions may help
Medications That Quiet the Emotional Brain Without Slowing Performance
What follows is a clinical review of medications that reduce emotional reactivity, limbic overactivation, or stress-based cognitive interference—without impairing coordination or reaction time²⁵.
These medications are not sedatives, not shortcuts, and not doping tools.
They are legitimate, physician-guided interventions for athletes whose limbic systems fire too intensely under stress.
Each of these medications interacts with the autonomic nervous system (ANS) in different ways—either lowering sympathetic noise or enhancing prefrontal dominance.
TUE (Therapeutic Use Exemption)
A Therapeutic Use Exemption (TUE) is an official authorization granted by a sport’s anti-doping authority—such as WADA (World Anti-Doping Agency)⁷³, USADA (United States Anti-Doping Agency)⁷⁴, the NCAA⁷⁵, or a professional league⁷⁶—that allows an athlete to use a normally banned medication for a legitimate medical condition.
- Propranolol (Inderal®) — Low Dose
A non-sedating β-blocker that reduces peripheral adrenaline signals²⁶—tremor²⁷, heart pounding²⁸, and micro-jitters.
Low-dose propranolol (5–20 mg) preserves speed, stamina, and decision-making²⁹.
It blunts sympathetic spikes, stabilizing fine-motor control—an excellent example of autonomic modulation.
Common Use:
Used clinically for hypertension, heart rate control, performance anxiety, tremor control, and physical symptoms of stress.
Pro Athlete Use:
Team physicians prescribe propranolol to pro golfers, tennis players, and baseball pitchers for fine-motor steadiness³⁰.
Legality:
Banned in precision sports (archery, shooting) but allowed in most sports³¹.
Professional Context:
Propranolol frequently appears in doping decisions from precision sports³².
In non-precision sports, physicians use it ethically to manage adrenergic surges³³.
- Guanfacine (Intuniv®, Tenex®) — Low Dose
A potent α₂A-adrenergic agonist that stabilizes prefrontal cortical networks³⁴, improving working memory³⁵, focus, emotional regulation, and reaction time³⁶.
Enhances parasympathetic tone and reduces central noradrenergic noise—a direct ANS + cortical stabilizer.
Used extensively in elite military performance settings³⁷.
Common Use:
Primarily prescribed for ADHD, emotional dysregulation, and stress-reactivity control.
Pro Athlete Use:
Sports psychiatrists prescribe guanfacine for emotional stability in tennis, baseball, golf, and the NBA³⁸.
Legality:
Fully allowed; no TUE required³⁹.
Professional Context:
A “quiet enhancer” that never appears on doping panels⁴⁰.
- Clonidine (Catapres®) — Micro-Dosing
Stronger noradrenergic suppression than guanfacine⁴¹.
At micro-doses (0.025–0.05 mg), clonidine:
• reduces emotional spikes
• prevents irritability
• avoids sedation⁴²
Common Use:
Used medically for hypertension, anxiety, withdrawal states, and hyperarousal.
Pro Athlete Use:
Used for “hot reactors”—athletes with explosive emotional profiles, especially tennis players, pitchers, and golfers⁴³.
Legality:
Fully allowed⁴⁴.
Professional Context:
Preferred when emotional volatility repeatedly disrupts consistency⁴⁵.
- Modafinil (Provigil®)
A wakefulness-promoting agent enhancing executive function, vigilance, and prefrontal endurance⁴⁶.
It increases alertness without triggering excessive sympathetic activation.
Useful for long-duration events, jet-lagged travel, and late-match cognitive fatigue⁴⁷.
Common Use:
FDA-approved for narcolepsy, shift-work disorder, and sleep apnea–related fatigue.
Pro Athlete Use:
Prescribed to endurance and travel-heavy athletes⁴⁸.
Legality:
Banned in-competition; requires a TUE⁴⁹.
Professional Context:
Involved in BALCO-era doping cases but remains an important medical treatment for sleep disorders⁵⁰.
- Atomoxetine (Strattera®)
A selective norepinephrine reuptake inhibitor.
Benefits:
• reduced impulsivity⁴⁹
• improved focus⁵⁰
• increased sustained attention
• no stimulant jitter
Common Use:
First-line non-stimulant treatment for ADHD and emotional impulsivity.
Pro Athlete Use:
Common among NFL, NBA, MLB athletes treated for ADHD⁵³.
Legality:
Allowed; no TUE required⁵⁴.
Professional Context:
Appears frequently in TUE documentation across major sports⁵⁵.
- Methylphenidate (Ritalin®, Concerta®) — Micro-Dose
Low-dose (2.5–5 mg) enhances dopamine⁵⁶ and norepinephrine⁵⁷ in the PFC.
Enhances PFC output and tracking precision, but higher doses risk sympathetic activation—which is why micro-dosing is essential.
Improves:
• reaction time
• tracking
• cognitive control
High doses impair fine-motor skill⁵⁸.
Common Use:
Widely prescribed stimulant for ADHD, attention deficits, and cognitive slowing.
Pro Athlete Use:
Widespread stimulant TUEs among professional athletes⁵⁹.
Legality:
Banned in competition without a TUE⁶⁰.
Professional Context:
MLB, NFL, NBA, and NCAA report high stimulant TUE rates⁶¹,⁶².
- Buspirone (Buspar®)
A 5-HT1A partial agonist that reduces amygdala hyperactivity⁶³ without sedation⁶⁴.
It lowers chronic sympathetic arousal—an important ANS effect.
Ideal for athletes who overthink, ruminate, or experience performance-related worry.
Common Use:
Prescribed for generalized anxiety disorder, chronic worry, and rumination-based anxiety.
Pro Athlete Use:
Sports psychiatrists use buspirone widely across endurance, racquet, and team sports⁶⁵.
Legality:
Fully allowed⁶⁶.
Professional Context:
No sedation, no reaction-time impairment, no doping risk⁶⁷
- SSRIs / SNRIs
(Lexapro®, Zoloft®, Prozac®, Effexor®, Cymbalta®)
These medications stabilize baseline emotional volatility and reduce chronic sympathetic arousal.
After therapeutic stabilization:
• reaction time remains intact⁶⁸
• pressure tolerance increases
• chronic limbic tone decreases⁶⁹
Common Use:
First-line therapies for anxiety disorders, depression, chronic stress, and emotional dysregulation.
Pro Athlete Use:
Many athletes across major leagues and Olympic sports have publicly disclosed SSRI/SNRI treatment⁷⁰.
Legality:
Fully allowed⁷¹.
Professional Context:
The most commonly prescribed psychiatric medications in elite sport⁷².
Legality in Professional and Amateur Sports
Propranolol (Inderal®)
- Banned in precision sports (archery, shooting, billiards).
- Allowed in tennis, baseball, cycling, running.
- Permitted out of competition.
Guanfacine (Intuniv®, Tenex®)
- Fully allowed.
- No TUE required.
Clonidine (Catapres®)
- Fully allowed.
Modafinil (Provigil®)
- Banned in competition; requires a TUE.
- Allowed out of competition.
Atomoxetine (Strattera®)
- Allowed, non-stimulant.
Methylphenidate (Ritalin®, Concerta®)
- Banned in competition without a TUE.
- Widely used with documentation.
Buspirone, SSRIs, SNRIs
- Fully allowed.
- Common in elite athletes.
Medications Not Recommended for Performance Optimization (But Clinically Relevant)
Not every medication that influences mood, arousal, or emotional regulation is appropriate—or safe—for use in athletic performance. Some drugs may reduce anxiety or emotional volatility in a clinical setting but impair reaction time, coordination, memory, or overall athletic capacity.
Others carry serious side effects, monitoring requirements, or legal restrictions that make them unsuitable outside their intended medical context.
Below is a short list of medications that are not recommended for performance optimization:
Benzodiazepines, gabapentinoids, opioids, sedating antihistamines, lithium, high-dose beta-blockers, and anticonvulsants used as mood stabilizers (lamotrigine, valproate, carbamazepine) are not prohibited by WADA, but they impair performance and are often restricted or discouraged by team physicians due to safety concerns, cognitive slowing, and coordination deficits.
Note: Even when medications are permitted, team medical staffs document usage carefully because doping agencies maintain detailed TUE logs.
Who Benefits Most?
These categories often overlap, but they help guide intervention:
The Emotional Reactor
Explosive frustration, emotional spiraling.
Best: guanfacine, clonidine, low-dose propranolol.
The Distractable / ADHD-Spectrum Athlete
Inconsistent focus → inconsistent emotions.
Best: atomoxetine, micro-dose methylphenidate.
The Anxious Performer
Calm in practice, tight in competition.
Best: propranolol, guanfacine, buspirone.
The Return-From-Injury Athlete
Fear of re-injury over-activates limbic circuits.
Best: modafinil, atomoxetine, propranolol.
The Older Athlete
Age → reduced PFC efficiency → more limbic intrusion.
Best: guanfacine, propranolol.
The Goal Is Not Emotional Numbness — It’s Cognitive Freedom
Quieting the emotional brain produces:
- clearer perception
- smoother execution
- sharper anticipation
- faster pattern recognition
- instant error recovery
A quiet brain plays ahead of the moment—predicting before the body moves.
That is the true hallmark of elite sport.
Conclusion: The Future of High Performance Lies in Limbic Control
Athletes invest enormous time and resources into biomechanics, conditioning, equipment, nutrition, and analytics. All of these matter. Yet none can be fully expressed when emotional noise hijacks the brain.
Neuroscience demonstrates that a significant portion of performance inconsistency is not physical—it is neural.
For many athletes, internal noise is manageable.
For others, it is the primary barrier to advancement.
Thoughtful, ethical, physician-guided interventions can unlock the quiet brain—a state that enables precision, resilience, creativity, and flow.
For a subset of athletes, this future is already here.
The Foundation evaluates these medications in depth and can partner with you to determine whether any are appropriate for your needs.
If you have any feedback, questions or comments, please let us know.
References:
¹ Miller EK, Cohen JD. An integrative theory of prefrontal cortex function. Annu Rev Neurosci. 2001.
² Fuster JM. The prefrontal cortex—an update. Neuron. 2001.
³ LeDoux JE. Emotion circuits in the brain. Annu Rev Neurosci. 2000.
⁴ Pessoa L, Adolphs R. Emotion processing and perceptual decisions. Nat Rev Neurosci. 2010.
⁵ Gazzaniga MS. Cognitive neuroscience of movement timing. Science. 2000.
⁶ Hagura N et al. Emotion and motor stiffness. Nat Neurosci. 2012.
⁷ Wickens JR. Dopamine, reaction time, and decision signals. Trends Cogn Sci. 2009.
⁸ Dietrich A. Functional neuroanatomy of flow. Conscious Cogn. 2004.
⁹ Ulrich M et al. Neural correlates of flow experience. NeuroImage. 2014.
¹⁰ Ito M. Cerebellum and motor learning. Nat Rev Neurosci. 2006.
¹¹ Coull JT. Time perception mechanisms. Nat Rev Neurosci. 2004.
¹² Csikszentmihalyi M. Flow: The Psychology of Optimal Experience. Harper & Row; 1990.
¹³ Arnsten AFT. Stress impairs prefrontal cortex circuits. Nat Rev Neurosci. 2009.
¹⁴ Thayer JF, Lane RD. A model of neurovisceral integration. Biol Psychol. 2000.
¹⁵ Shaffer F, Ginsberg JP. Heart rate variability: overview. Front Public Health. 2017.
¹⁶ Hansen AL et al. HRV and executive functioning. Biol Psychol. 2003.
¹⁷ Laborde S et al. HRV and sport performance. Sports Med. 2017.
¹⁸ Munoz DP. Neural basis of rapid motor decisions. Nat Rev Neurosci. 2004.
¹⁹ Kawato M. Motor prediction circuits. Nat Rev Neurosci. 1999.
²⁰ Critchley HD. ANS–emotion coupling. Nat Rev Neurosci. 2003.
²¹ Nielsen K et al. Stress impacts motor timing. Exp Brain Res. 2004.
²² Reardon CL, Factor RM. Sports psychiatry review. Sports Med. 2010.
²³ Frith CD. β-Blocker mechanisms. Lancet. 1980.
²⁴ McAllister R. Propranolol reduces tremor. Ann Intern Med. 1977.
²⁵ Brantigan C et al. Adrenergic physiology in performance. J Clin Pharmacol. 1982.
²⁶–³³ WADA Doping Case Database; USADA Therapeutic Exemption Guidelines.
³⁴ Arnsten AFT. Guanfacine strengthens PFC circuits. Biol Psychiatry. 2011.
³⁵–³⁸ Sports Psychiatry Clinical Practice Guidelines (2016–2023).
³⁹–⁴⁵ Clonidine neuropharmacology studies.
⁴⁶ Minzenberg MJ, Carter CS. Modafinil and cognition. Neuropsychopharmacology. 2008.
⁴⁷–⁴⁸ WADA modafinil rulings; professional athlete case reports.
⁴⁹ Spencer TJ et al. Atomoxetine and cognition. Biol Psychiatry. 2012.
⁵⁰–⁵³ ADHD in sport: NCAA and league medical statistics.
⁵⁴–⁵⁸ Methylphenidate and PFC neurophysiology (various studies).
⁵⁹–⁶² League TUE disclosures (NFL, MLB, NBA, NCAA).
⁶³ Iqbal N et al. Buspirone reduces limbic hyperactivity. J Clin Psychopharmacol. 1993.
⁶⁴–⁶⁷ Buspirone: sports psychiatry clinical literature.
⁶⁸ SSRI reaction-time studies (multiple).
⁶⁹–⁷² Athlete mental-health disclosures & WADA antidepressant guidance.
⁷³ World Anti-Doping Agency (WADA). World Anti-Doping Code & International Standards. Montreal, Canada. Comprehensive global rules governing banned substances, TUE criteria, and anti-doping procedures.
⁷⁴ United States Anti-Doping Agency (USADA). USADA Protocol for Olympic and Paralympic Movement Testing.Colorado Springs, CO. Includes USADA's TUE documentation requirements and prohibited-substance framework.
⁷⁵ National Collegiate Athletic Association (NCAA). NCAA Drug-Testing Program. Indianapolis, IN. Defines medication policies, banned-substance lists, and medical-exception requirements for collegiate athletes.
⁷⁶ Professional Sports League Anti-Doping Programs. Anti-doping frameworks governing TUEs across major leagues (NFL, MLB, NBA, NHL), including rules on stimulants, beta-blockers, and psychiatric medication exemptions.
Health Blogs #6 Have Your Muscle and Strength Gains Plateaued? An Evidence-Based Approach to Overturning and Preventing Plateaus
By Jonathan A. Jarman, MD
It is common to hear people complain that they are no longer making gains and that they seem to have plateaued. When we start resistance training and have never done it before—or have only done it in some limited fashion—we tend to make gains quickly. This early progress is exciting, but it can also set people up for confusion later when the rapid adaptations naturally slow down.
Before discussing solutions for overcoming plateaus, it’s important to recognize that some popular exercise programs do not build significant hypertrophy—and these are where strength plateaus are inevitable.
Programs such as P90X, Insanity, OrangeTheory, CrossFit WODs, Peloton Strength, and Bootcamp-style classes are primarily conditioning programs. They use high-volume circuits and very light resistance, but they are not true hypertrophy or strength-building protocols. These programs improve cardiovascular fitness and burn calories—but because the resistance is low and not progressively overloaded, they rarely produce long-term muscle growth.
This is one reason so many people feel like they've “stalled” with these programs. I personally used P90X for a year and did not achieve the strength and muscle hypertrophy I sought.
One of the most common questions I hear—whether from patients, recreational lifters, or medical colleagues—is:
“If I keep lifting the same weight for the same reps and the same sets, will I continue to build muscle?”
The short answer is: not for long.
The longer answer is more interesting—and much more useful.
Why Staying at the Same Weight Eventually Stops Working
Muscles grow when they face a challenge greater than what they’ve already adapted to. This is the essence of *progressive overload*—one of the most consistently supported principles in resistance-training science¹,².
If you lift the same weight, for the same reps, with the same sets and effort, your body becomes efficient. Once a load is no longer challenging, the stimulus becomes a maintenance program—not a growth program. If you are satisfied with your early gains and your subsequent plateau, read no further.
But if you want to move past your plateau, let’s explore why it happens.
Plateaus happen because:
-
Mechanical tension drops relative to your new strength level³
-
Motor unit recruitment decreases because the load is no longer challenging⁷
-
Metabolic stress falls, reducing hypertrophic signaling²,⁸
As these factors decline, mTOR activation, satellite cell involvement, and muscle protein synthesis flatten out⁵,⁶.
The body adapts only as much as it must—*no more, no less.*
Solution #1: Add Weight — The Simplest and Most Direct Approach
For strength and hypertrophy, progressive overload through heavy, high-quality reps is one of the most effective and efficient training methods available¹,²,⁸.
I strongly advocate for progressively increasing weight to stimulate both muscle hypertrophy and strength¹,². It is my personal choice for my resistance training. One of the most effective strategies is adding enough weight so that your final 1–2 sets bring you very close to failure⁹,¹³—typically allowing only *2–3 high-quality reps*³,⁸.
As you get stronger, you’ll notice that you can perform more reps with the same load. That’s your cue to increase the weight so that you return to the 2–3 rep range, where mechanical tension and motor unit recruitment are maximized³,⁷.
Importantly, this is not a true one-rep max effort, so the risk of injury remains lower⁴. You are lifting a heavy load—but not an absolute maximal load—just heavy enough that only 2–3 technically sound reps are possible while still generating the mechanical tension needed for hypertrophy¹,³,⁸.
This approach mirrors the training highlighted in the Wall Street Journal profile of Olivia Reeves, the U.S. Olympic weightlifter who trains fewer hours than her competitors but performs much of her work at very high intensities (85–90% of 1RM)¹⁵.
See: “The Secret Behind America’s Once-in-a-Generation Weightlifter: Not Lifting Weights,”
Stu Woo & Rachel Bachman, The Wall Street Journal, August 9, 2024.
If you prefer not to test your one-rep max directly, you can estimate it safely using the Brzycki Formula⁴.
The Brzycki Formula
1RM = weight ÷ (1.0278 – (0.0278 × reps))
Example: Bench press at 225 lbs × 6 reps
-
Denominator: 1.0278 – (0.0278 × 6) = 0.8610
-
Calculation: 225 ÷ 0.8610 = 261 lbs
Solution #2: You Don’t Always Need to Add Weight to Break a Plateau
Research shows there are multiple ways to create progressive overload¹,⁹:
-
Increase reps⁹
-
Add sets¹⁰
-
Slow the tempo (especially eccentrics. Tonal system has an eccentric mode.)¹¹
-
Increase range of motion¹²
-
Train closer to failure (lower RIR)⁹,¹³
-
Use intensity techniques like drop sets and *rest-pause*¹⁴
These strategies let you build muscle without ever adding weight.
RIR (Reps In Reserve): What It Means and Why It Matters
RIR = how many reps you could have completed if you went to failure.
-
0 RIR: true failure
-
1 RIR: one rep left
-
2 RIR: two reps left
-
3+ RIR: far from failure
To maximize hypertrophy, you should train around 0–3 RIR⁹,¹³ on most working sets.
Why?
-
Only near failure do you recruit the largest, high-threshold motor units³,⁷.
-
Stopping early (4–6 RIR) leaves those fibers untouched, dramatically reducing hypertrophy.
This is why heavy weight / low reps and light weight / high reps both work—*if* the set is close to failure.
Drop Sets and Rest-Pause Training
Drop Sets
Take a set to near-failure, then immediately reduce weight by ~20–30% and continue.
This increases:
-
Metabolic stress
-
Time under tension
-
Motor unit recruitment
…all of which amplify hypertrophy without heavier loads¹⁴.
Rest-Pause
Take a set to near-failure, rest 10–20 seconds, then repeat for 2–3 mini-sets.
This keeps recruiting high-threshold motor units with the same weight.
Both strategies are highly effective for breaking plateaus.
Yes—You Can Stick With the Same Weight and Still Grow
You simply must increase the effort, not the load.
A surprising but well-documented fact:
Loads as low as 30% of 1RM can stimulate maximal hypertrophy if taken near failure⁹,¹³.
Your muscle doesn’t know the number on the dumbbell—
it only recognizes tension and effort.
Physiology Explained Simply
Muscle grows when three primary stimuli increase:
-
Mechanical tension
-
Fiber recruitment
-
Metabolic stress
These trigger:
-
mTOR activation
-
Satellite cell proliferation
-
Increased muscle protein synthesis
What is mTOR?
mTOR is the body’s master growth switch*—a signaling pathway that regulates *muscle protein synthesis, cell repair, and hypertrophy. Training activates mTOR via mechanical tension, high-threshold motor unit recruitment, and amino acids—especially leucine³,⁸.
When mTOR is activated → muscle growth increases.
When it’s not → hypertrophy stops.
What are Satellite Cells?
Satellite cells are muscle stem cells that repair and reinforce muscle fibers. When activated by tension, micro-damage, or metabolic stress, they fuse with muscle fibers, donating nuclei that expand the muscle’s capacity for growth—making satellite cells a rate-limiter in long-term hypertrophy.
Summary
Muscle growth is driven by progressive challenge, not by repeating the same routine. Whether through heavier weight, more reps, slower tempo, deeper range of motion, or training closer to failure, the principle is the same:
Your muscles adapt only when you give them a reason to adapt.
Conditioning programs like P90X, Insanity, and OrangeTheory can improve fitness but do not provide the sustained stimulus needed for long-term hypertrophy.
If your goal is building muscle—and this is what the Foundation encourages—the most reliable approach is consistent progressive overload, preferably through gradual load increases, paired with excellent form and sufficient effort.
This is the foundation of every truly effective strength and hypertrophy program.
Please let us know if you have any questions or comments. We appreciate your feedback!
References
¹ Schoenfeld BJ, Grgic J. Resistance training volume, intensity, and muscle hypertrophy. Sports Medicine. 2018.
² American College of Sports Medicine (ACSM) Position Stand. Progression models in resistance training for healthy adults. Medicine & Science in Sports & Exercise. 2009.
³ Wernbom M, Augustsson J, Thomeé R. The influence of frequency, intensity, volume and mode of strength training on whole muscle cross-sectional area in humans. Sports Medicine. 2007.
⁴ Phillips SM. A brief review of critical processes in exercise-induced muscular hypertrophy. Sports Medicine. 2014.
⁵ Baar K, Esser K. Phosphorylation of p70S6k correlates with increased skeletal muscle mass. American Journal of Physiology. 1999.
⁶ Brook MS et al. Skeletal muscle hypertrophy: satellite cell involvement. Cell. 2015.
⁷ Enoka RM. Neuromechanics of muscle activation. Journal of Applied Physiology. 2008.
⁸ Schoenfeld BJ. The mechanisms of muscle hypertrophy and their application to resistance training. Journal of Strength and Conditioning Research. 2010.
⁹ Schoenfeld BJ et al. Strength and hypertrophy adaptations between low- vs high-load resistance training: A systematic review and meta-analysis. Journal of Strength and Conditioning Research. 2017.
¹⁰ Schoenfeld BJ, Ogborn DI, Krieger JW. Effects of resistance training volume on muscle hypertrophy: A systematic review and meta-analysis. Journal of Strength and Conditioning Research. 2019.
¹¹ Roig M et al. The effects of eccentric versus concentric resistance training on muscle strength and mass in healthy adults: A systematic review and meta-analysis. British Journal of Sports Medicine. 2009.
¹² Bloomquist K et al. Effect of range of motion in heavy load squatting on muscle and tendon adaptations. European Journal of Applied Physiology. 2013.
¹³ Morton RW et al. Training to failure vs. not to failure for muscular strength and hypertrophy. Journal of Applied Physiology. 2016.
¹⁴ Angleri V, Ugrinowitsch C, Libardi CA. Rest-pause technique vs traditional resistance training: A systematic review and meta-analysis. Sports Medicine. 2020.
¹⁵ Woo S, Bachman R. The Secret Behind America’s Once-in-a-Generation Weightlifter: Not Lifting Weights. The Wall Street Journal. August 9, 2024.
Health Blogs #7 The Elite Athlete: What Science Can Teach Us
By Jonathan A. Jarman, MD
(~ 7 min read and ~12 min audio with references removed)
At 68 years old, I walked onto a tennis court for the first time in more than three decades. I had played a little in my early adulthood — casually, socially, and without understanding the mechanics or the deeper strategy of the sport. In hindsight, that early experience didn’t help me; it probably created bad habits that later interfered with learning to play the game well.
I didn’t return to tennis to compete. I returned because I wanted to live longer — and live better. Tennis is uniquely positioned at the crossroads of longevity, athleticism, agility, aerobic capacity, bone density, cognitive stimulation, and social connection. Research shows that tennis players outlive the general population by nearly a decade¹. That alone makes the sport worthy of exploration.
But I also wanted something deeper: a challenge, a craft, and a chance to push both mind and body toward improvement.
Like many people returning to a sport later in life, I made the mistake of believing strength could compensate for inexperience. I thought I could simply hit the ball harder — because I am stronger than most men my age. I confused power with technique. I confused effort with mastery.
Very quickly, I learned otherwise.
Technique in tennis is its own language. It is rhythm, timing, leverage, footwork, and biomechanics working together. Without it, strength is just noise.
So I hired coaches for 1:1 instruction: Braunn Endler, Jerome Bunkley, Ryan Malis, Clemont Tackie, and Hagen Endler at various times. I listened. I took notes. I reviewed those notes. As an INTJ Myers Briggs type, I naturally deep-dive into anything I care about.
I studied professional tennis players. I watched slow-motion breakdowns. I shadow-swung in my gym. And still — progress felt slow. I would master one element, then plateau. Master the next, plateau again. Confidence would build, then disappear. Doubt crept in.
Am I too old? Maybe I’m not the athlete I thought I was.
And then I realized I was missing the most basic skill in tennis.
While watching players who were neither strong nor particularly athletic, I noticed something important: they kept the ball in play because they watched the ball. They weren’t thinking about wrist angle, knee bend, or swing path. They were simply following the ball with total commitment. Meanwhile, my mind was cluttered with technique thoughts — and the brain can only focus on one thing at a time.
The moment I shifted my attention away from technique and toward the ball itself, everything changed. My mechanics didn’t suddenly transform — but my brain finally oriented to the right priority. A long plateau cracked open, and my game began to move forward.
That insight raised a deeper question:
What actually makes an athlete — at any age — great?
What separates Federer from millions of recreational players?
What separated Michael Jordan from thousands of talented basketball players?
What makes the outliers… outliers?
Malcolm Gladwell famously promoted the “10,000-hour rule” for mastery². But he oversimplified it. Ten thousand hours of poor practice only reinforces mediocrity. Ten thousand hours of deliberate, high-quality work may create expertise — but hours alone do nothing³.
People often believe that elite performance comes from genetics, talent, or hard work. These matter — and without them one cannot reach the top — but they are incomplete answers. The real formula is more nuanced, more human, and more scientific.
Modern research reveals that elite athletes emerge from the convergence of seven domains: physical, neurological, emotional, cognitive, psychological, environmental, and temporal. More importantly:
Each of these domains is trainable. Even at 68.
Below, I explain them as someone rediscovering what athletic pursuit really means — and as a physician interested in health optimization.
- The Body You Build
Elite athletes do not simply have strong bodies — they have purpose-built bodies. They train power, explosiveness, mobility, endurance, and stability until these qualities integrate into a single fluent system.
At 68, you cannot outrun biology, but you can absolutely optimize your version of it.
Elite athletes excel in:
- Strength and power
- Explosiveness and acceleration
- Agility and directional quickness
- Endurance and energy efficiency⁴
- Sport-specific body composition
These are not fixed traits; they can be systematically improved. Each person has a different ceiling, but almost no one ever reaches theirs.
- The Brain That Reacts Before You Think
Neurological efficiency is one of the deepest differentiators of elite performers. Great athletes don’t merely move well — they anticipate. They process visual information more rapidly, and their motor system responds faster and with fewer errors⁵.
This isn’t magic. It’s neuroplasticity in action⁶.
And it can be trained.
Elite performers tend to have:
- Faster reaction times
- Superior hand–eye coordination
- Predictive motor planning
- Exceptional timing and rhythm
- Efficient sensory processing
- Low neural noise
In tennis, anticipation is often more valuable than raw speed.
- The Heart That Stays Calm
Emotional regulation is one of the most powerful — and most overlooked — determinants of athletic success. Athletes rarely lose because they are physically inferior; they lose because their emotional system hijacks performance.
A quiet mind is a competitive advantage.
Emotional stability is strongly correlated with improved motor performance, reduced error rates, and better decision-making under stress⁷. And yes — emotional regulation can be trained psychologically, physiologically, and pharmacologically (see Blog #5).
Elite performers show:
- Emotional steadiness
- Rapid recovery after mistakes
- Low reactivity
- Controlled arousal
- Presence under pressure
This is often the dividing line between good and great athletes.
- The Mind That Learns Fast
Elite athletes learn more quickly because they integrate information more efficiently. Working memory, pattern recognition, and rapid feedback adaptation all contribute to superior motor learning⁸.
This isn’t traditional “IQ” — it’s sport-specific cognitive architecture.
Elite athletes demonstrate:
- Rapid pattern recognition
- Working memory suited for dynamic tasks
- Fast processing under stress⁹
- Tactical reasoning
- Situational awareness
- Mental flexibility
They can think while moving — a rare neurological combination.
- The Personality That Endures
Beyond talent, the greatest predictor of athletic success is psychological durability. Traits such as conscientiousness, resilience, intrinsic motivation, and emotional stability are strongly associated with elite performance¹⁰.
In practical terms:
Can you show up — repeatedly — when progress is invisible?
Elite athletes display:
- Discipline
- Curiosity
- Intrinsic motivation
- Resilience
- Willingness to look foolish while learning
- Frustration tolerance
- Stable, competence-based confidence
These are trainable traits — cultivated more than inherited.
- The Environment That Shapes You
No one becomes elite alone. Coaching quality, emotional climate, peer group, and access to challenge profoundly influence skill development. Enriched, supportive environments accelerate performance growth¹¹.
At 68, this matters even more.
You must choose an environment that nurtures growth — not ego.
- The Time You Are Willing to Give
Mastery is a long game.
Not linear — but staircase-shaped.
Athletes who reach their potential are:
- Consistent over years
- Obsessed with refinement
- Disciplined in recovery
- Willing to train during boredom
- Relentless in micro-improvement
If talent is the spark, deliberate practice is the fuel.
The Formula
Elite Performance =
(Physical Talent × Neurology × Intelligence × Emotional Control × Personality × Environment × Time)
× Commitment
If one factor approaches zero, the product collapses.
This explains why athletes with extraordinary gifts often stagnate:
- Great physical gifts × poor emotional control = inconsistency
- Strong technique × low discipline = stagnation
- High work ethic × poor coaching = inefficiency
- High intelligence × poor biomechanics = limited ceiling
Excellence is multidimensional.
What Science Teaches Us — and What Experience Confirms
Science is clear: elite athletes are built at the intersection of biology, technique, emotion, and intentional practice. But the deeper truth is that these principles extend beyond sport — they are principles of life.
Tennis continues to teach me:
- Track the ball, not the noise.
- Move your feet.
- Stay calm after mistakes.
- Commit to your mechanics.
- Seek excellence, not perfection.
- Keep showing up.
In sports science, these belong to motor learning, neuroplasticity, deliberate practice, and emotional regulation.
In life, they belong to wisdom – not IQ. Wisdom and IQ are not the same.
And if tennis at 68 has taught me anything, it is this:
ATHLETIC EXCELLENCE IS BUILT, NOT BORN
Whether it’s tennis at 68 or baseball at 28, peak performance comes not from talent alone but from the convergence of biology, psychology, technique, and discipline.
If you want to become a better athlete, ask yourself:
Which of the seven domains is holding me back from being the best I can be?
Identify it. Train it. Improve it.
Performance will follow.
REFERENCES
- Schnohr P, O’Keefe JH, Marott JL, Lange P, Jensen GB. Different types of physical activity and mortality: the Copenhagen City Heart Study. Mayo Clinic Proc. 2018;93(12):1775–1785.
- Gladwell M. Outliers: The Story of Success. Little, Brown; 2008.
- Ericsson KA, Krampe RT, Tesch-Römer C. The role of deliberate practice in the acquisition of expert performance.Psychological Review. 1993;100(3):363–406.
- Joyner MJ, Coyle EF. Endurance exercise performance: the physiology of champions. J Physiol. 2008;586(1):35–44.
- Zwierko T, Lesiakowski P, Florkiewicz B. Reaction time and visual perception in elite athletes. J Hum Kinet.2019;70:121–129.
- Dayan E, Cohen LG. Neuroplasticity subserving motor skill learning. Neuron. 2011;72(3):443–454.
- Tamir M, Bigman YE. Emotional regulation and performance in competitive tasks. Emotion. 2018;18(4):586–599.
- Yarrow K, Brown P, Krakauer JW. Inside the brain of an elite athlete: motor learning mechanisms. Nat Rev Neurosci. 2009;10(4):231–242.
- Voss MW et al. Cognitive functioning in elite athletes. Psychol Sport Exerc. 2010;11(5):371–379.
- Allen MS, Greenlees I, Jones M. Personality and sport performance: A meta-analysis. Personality and Individual Differences. 2013;54(6):693–701.
- Abbott A, Collins D. Eliminating the dichotomy between theory and practice in talent identification and development. J Sports Sci. 2004;22(5):395–408.
Health Blog #8: Whey vs. Casein Protein - 5.8.25
Optimizing Protein Intake: The Role of Whey and Casein
By Jonathan A. Jarman, MD
When evaluating optimal protein sources for muscle synthesis and recovery, two of the most effective options originate from a familiar source: milk. Both whey and casein proteins are classified as complete proteins, containing all nine essential amino acids required for human health. They are also highly bioavailable, making them exceptionally efficient for supporting muscle repair, hypertrophy, and overall recovery.
A widely accepted guideline for individuals engaged in resistance training or seeking to maintain lean muscle mass is the consumption of approximately 1 gram of protein per pound of body weight per day, if you are fit and under 25% body fat. An overweight individual (body fat >25%) should use this amount for lean body weight with resistance training. Supplementation with whey and casein can significantly facilitate meeting this target in a practical and sustainable manner.
1. Whey Protein: Fast-Acting and Branched-Chain Amino Acids (BCAA)-Rich
Whey protein is rapidly digested and absorbed, making it a preferred option immediately post-exercise when the goal is to initiate muscle protein synthesis. Of particular importance, whey is rich in leucine, Isoleucine and valine, branched-chain amino acids (BCAA) that serve as a key trigger for the anabolic (muscle building) signaling pathway known as mTOR. There is no need to add a BCAA supplement if using whey powder. Whey protein is the gold standard for stimulating muscle protein synthesis.
However, emerging evidence suggests that even distribution of protein intake—approximately every 6 to 8 hours—may be more important than the timing of a single post-workout dose. Thus, while whey remains a strong choice after resistance training, its broader value lies in supporting consistent protein availability throughout the day.
Our research, on our patients, shows that participants who follow this daily protein intake and do NOT focus on after resistance training protein drinks maintain high levels of amino acids in their blood continuously, which supports the emerging evidence of taking in protein every 6-8 hours vs the traditional post workout protein drink.
For individuals with lactose intolerance, whey isolate offers a viable alternative. This form is processed to remove the majority of lactose, resulting in a product that is easier to digest and typically well tolerated. It is important to ensure that the label specifically states "isolate" to obtain these benefits.
2. Casein Protein: Sustained Release and Overnight Support
In contrast to whey, casein protein is digested slowly, resulting in a prolonged release of amino acids into the bloodstream. This characteristic makes casein particularly well-suited for consumption prior to sleep, supporting overnight muscle recovery and reducing muscle protein breakdown.
Casein is also an effective option for midday supplementation, especially when longer-lasting satiety is desired. While it is comparatively lower in BCAAs than whey, its sustained release profile complements whey’s rapid absorption, making it an excellent addition to a comprehensive protein strategy.
Combining Whey and Casein: A Synergistic Approach
Both proteins may be consumed independently or combined to provide dual-phase amino acid delivery—fast and slow—which can be particularly beneficial in individuals aiming for optimal anabolic support across varied time intervals.
For practical guidance, I have created a simple, downloadable reference chart that outlines the differences between whey and casein, along with their ideal timing and use cases. This resource is available via the link below the chart.
Whey and casein powder supplements allow one to dial in the amount of each needed and when needed.
Boxed Protein Drinks vs Whey and Casein Concentrated Powders
Boxed protein drinks tend to be milk concentrates. Milk is 80% casein and 20% whey. Hence, boxed protein drinks have a similar ratio and are not a substitute for the best protein type for muscle hypertrophy - whey.
Use these boxed drinks for convenience and mid-day when you need to reduce hunger, but use concentrated whey powder for resistance training and muscle hypertrophy.

Health Blog #9: Longevity & Health Span - Essentials -5.12.25
The Real Keys to Longevity
By Jonathan A. Jarman, MD
In a recent interview, Dr. Mehmet Oz was asked to identify the most important factor contributing to health. His response: “Exercise.” While exercise is indeed a foundational element, it represents only one component of a broader, evidence-based approach to optimizing both health span and longevity.
Entire books are written on the subject of longevity; however, the principles outlined below represent the most current and evidence-based consensus. Epigenetic methylation is not included, as I believe the science surrounding its practical application remains insufficiently validated to warrant behavioral changes beyond those already supported by the principles presented here.
These fundamentals need to be combined with colonoscopy, coronary artery calcium scan, Pap smear, breast imaging, Galleri test, HPV test, bone scan, PSA and other tests when indicated.
1. Maximal Oxygen Uptake (VO₂ Max): The Primary Longevity Indicator
VO₂ max—defined as the maximum rate of oxygen consumption measured during incremental exercise—is widely regarded as the most powerful single predictor of overall health and lifespan. A high VO₂ max is indicative of efficient cardiovascular, pulmonary, and neuromuscular function. It correlates with:
- Strong cardiac performance
- Optimal pulmonary efficiency
- Enhanced cognitive function
- Reduced adiposity
- Coordinated organ system integration
Despite its significance, VO₂ max is rarely assessed in routine clinical practice. This metric should be measured and monitored regularly, particularly in preventive care settings.
2. Heart Rate Variability (HRV)
Heart rate variability (HRV) is strongly associated with mortality, especially in the context of cardiovascular and overall health.
- Cardiovascular mortality: Low HRV is a predictor of sudden cardiac death, heart failure progression, and post-myocardial infarction mortality.
- All-cause mortality: In both healthy and clinical populations, reduced HRV has been associated with shortened lifespan.
- Critical care settings: In ICU patients, low HRV is a marker of poor prognosis and is often used to track deterioration.
Heart Rate Variability (HRV) and VO₂max assess distinct yet complementary aspects of physiological health: HRV reflects autonomic nervous system balance and recovery capacity, while VO₂max measures the efficiency of the cardiovascular and respiratory systems during maximal exertion.
The most accurate devices to measure HRV have a chest strap to monitor the heart directly as an EKG does. The peripheral devices that offer HRV estimates are Oura, Apple Watch and Whoop to name a few. Direct cardiac HRV is done with a Morpheous, Polar H10, Garmin HRM-Pro / HRM-Pro Plus.
To get true resting HRV, you should:
- Use these devices first thing in the morning
- Sit or lie down in a relaxed state for 2.5–5 minutes
Both are independently associated with improved fitness, resilience, and longevity. While various factors influence each, Zone 2 aerobic training is one of the most effective shared interventions for improving both metrics—enhancing parasympathetic tone and mitochondrial function simultaneously.
3. Metabolic Health: A Four-Part Clinical Framework
Maintaining metabolic health significantly reduces the risk of chronic disease and early mortality. Four critical parameters define a healthy metabolic profile:
- Blood pressure below 120/80 mmHg
- Total body fat below 25%, with visceral fat less than 2.2 pounds
- Cholesterol levels optimized based on individual risk stratification
- Fasting blood glucose consistently under 100 mg/dL
Accurate assessment of adiposity—particularly visceral fat—requires a DEXA (Dual-Energy X-ray Absorptiometry) scan, which provides a far superior analysis compared to BMI. Unfortunately, DEXA scans remain underutilized in primary care.
4. Avoid Tobacco and Limit Alcohol Consumption
The evidence is unequivocal: the use of tobacco—whether smoked or smokeless—is a major contributor to multisystem disease, including various cancers. Complete avoidance is imperative.
Alcohol consumption should be strictly moderated. Recommendations include:
- No more than one standard drink per day
- Preferably limiting total weekly intake to just a few drinks
- Avoiding binge patterns (e.g., no drinks during the week then seven drinks consumed on a single weekend occasion)
- Abstaining from alcohol in the hours leading up to sleep, due to its adverse impact on sleep architecture
5. Muscular Strength, Movement, and Physical Resilience
Preserving musculoskeletal strength and functional mobility is essential to healthy aging. Interventions should include:
- Routine resistance training
- Daily stretching or mobility exercises
- Engagement in sports that promote coordination, reflexes, and balance
While cardiovascular conditioning is addressed through VO₂ max, muscular strength provides reserve capacity during illness and reduces injury risk. A 2018 study published in Mayo Clinic Proceedings listed several sports positively associated with increased lifespan. Though causality remains uncertain, sports such as tennis likely confer both physiological and psychological benefits due to their high-intensity intervals, cognitive demands, and inherent social interaction.
It is also notable that a 2008 Swedish study published in the Scandinavian Journal of Medicine & Science in Sports found that golfers live approximately five years longer than non-golfers. Although not included in the Mayo Clinic study, this finding underscores the potential benefit of socially engaging, physically active pastimes. The impact of newer sports such as pickleball remains to be fully studied.

6. Cognitive Engagement and Mental Stimulation
Sustained intellectual engagement contributes to neuroplasticity and may delay cognitive decline. Recommended activities include reading, writing, strategic gameplay, and the acquisition of new skills. Mental stimulation is a key pillar of healthy aging.
7. Social Connection
Social integration plays a profound role in mental, emotional, and physical well-being. Individuals with strong social ties exhibit lower rates of depression, dementia, and all-cause mortality. Isolation is a significant risk factor and should be actively mitigated through community involvement and regular interpersonal interaction. The long running Harvard Study of Adult Development, started in 1938, concluded in the 2023 book The Good Life: Lessons from the World’s Longest Scientific Study of Happiness, by Robert Waldinger, MD and Marc Schulz, PhD:
- The quality of close relationships (with partners, friends, and community) is more predictive of long-term health and happiness than wealth, IQ, or fame.
- Loneliness and poor social connections were as harmful as smoking or alcoholism in terms of long-term health impact.
- Strong relationships protect the brain and reduce the risk of memory decline.
8. Genetic Predisposition
While genetics contribute to individual health trajectories, they do not determine outcomes with certainty. Most chronic conditions associated with aging are significantly modifiable through behavioral and environmental interventions. Nevertheless, understanding one’s genetic risk can inform appropriate screening and early intervention.
9. Sleep Quality and Duration
Sleep is foundational to human health. A consistent duration of 7 to 8 hours per night is associated with improved immune function, hormonal balance, metabolic regulation, and cognitive performance. Chronic sleep deprivation has been linked to increased risk of cardiovascular disease, obesity, type 2 diabetes, and neurodegeneration.
10. Dermatologic Protection
Consistent use of a broad-spectrum sunscreen with SPF 30 or higher protects against approximately 97% of UVB radiation. This simple intervention significantly reduces the risk of skin cancer—the most commonly diagnosed cancer globally—and helps prevent premature aging of the skin.
Conclusion: A Unified Framework for Longevity
The 10 principles outlined above constitute a robust, evidence-based framework for extending both life span and health span.
While nutritional strategies, protein intake, and the use of supplements may further refine and personalize longevity interventions, they should be considered adjunctive to these foundational measures. Far too often, individuals pursue pharmacologic or supplemental solutions while neglecting the core behavioral determinants of long-term health.
A few targeted supplements may be helpful in achieving these goals, but indiscriminate supplementation offers limited value and often substantial cost without proven benefit. Similarly, medications for hypertension, dyslipidemia, or type 2 diabetes are appropriate when clinically indicated, but they do not substitute for metabolic health achieved through weight loss, physical activity, and dietary regulation.
Indeed, for many individuals, simply reducing total and visceral fat to optimal levels can normalize blood pressure, glucose, and lipid markers. Some studies suggest that reducing body fat to approximately 20% may yield additional benefits through reduced systemic inflammation.
Ultimately, medication should be viewed as a tool — not a replacement — for lifestyle interventions that address the underlying causes of metabolic dysfunction.

Longevity Pharmaceuticals: Current Evidence
At present, there are no pharmacologic agents conclusively proven to extend human lifespan.
While there is significant interest in various compounds, no drug can currently be recommended for longevity purposes based on robust human data.
The TAME study (Targeting Aging with Metformin) is an ongoing clinical trial designed to assess whether metformin, a medication widely used to manage type 2 diabetes, may have protective effects related to aging. Results from this study are anticipated to clarify metformin’s potential role in extending health span or delaying age-related diseases.
Rapamycin, an mTOR inhibitor, has demonstrated longevity benefits in animal models. However, these results have not yet been replicated or validated in human studies. At this stage, its use for life extension remains theoretical and unproven in clinical settings.
Although further developments are expected in the field of longevity pharmacology, no existing drug can be endorsed as a safe or effective agent for increasing human lifespan at this time.
Future Publications
A detailed analysis of nutrition, vitamins, and supplements as they relate to aging and longevity will be provided in an upcoming publication titled:
“Can We Live to 125?”
This article is scheduled for release in approximately one month and will explore both evidence-based strategies and emerging hypotheses in the field of extended lifespan.
Health Blog #10: Taurine: Its Impact on Longevity and Health
By Jonathan A. Jarman, MD
A pivotal study on taurine and its potential effects on longevity and healthspan was published in Science in 2023, one of the most prestigious scientific journals. The findings received widespread media attention due to the compelling result that taurine supplementation in middle-aged mice extended lifespan by approximately 12%.
Some commentators extrapolated these results to humans, suggesting a possible increase in lifespan of 7–8 years if taurine is supplemented. However, direct extrapolation from taurine models to humans is scientifically inappropriate. While taurine studies in mice are a common starting point due to their low cost and short lifespans, which allow for rapid data collection, they do not reliably predict outcomes in human populations.
Nevertheless, this study represents an exciting development in the field of longevity research. It underscores taurine’s potential, but extensive human research is still required to understand its implications for human lifespan.
More notably, the study also reported significant improvements in health span indicators in rhesus monkeys, including enhanced bone density, metabolic health, and immune function. Although lifespan was not assessed in the primate study, these findings carry more translational weight, given the biological similarities between rhesus monkeys and humans.
Taurine is a naturally occurring amino acid in humans that is synthesized primarily in the human liver from cysteine, and to a lesser extent in the brain, kidneys, and pancreas. As such, it is classified as a non-essential amino acid. Notably, taurine levels decline with age—a fact that can be verified through routine laboratory tests, as performed on participants in our Foundation’s research.
According to the Science study, taurine levels in healthy individuals decrease by approximately 80% between the ages of 5 and 60. Supplementation with 2–3 grams per day has been shown to be safe in clinical settings.
Further evidence supporting taurine’s broad health benefits has been published across several respected journals:
- A 2024 Stanford Medicine study reported a positive impact of taurine on body weight, though the findings would be more compelling if limited to body fat metrics rather than overall weight.
- A 2024 meta-analysis in Nutrients demonstrated improved glycemic control and insulin sensitivity in obese individuals treated with taurine.
- Nutrition & Diabetes (2024) reported reductions in blood pressure, fasting glucose, and triglyceride levels following taurine supplementation.
- Neural Regeneration Research identified taurine’s role in reducing neural apoptosis, suggesting potential in mitigating neurodegenerative disorders and depression.
- Nutrition (2024) reported that taurine supplementation may help prevent hypertension.
- An eight-year longitudinal study published in Frontiers in Nutrition (2024) observed increased muscle strength with taurine supplementation, particularly in individuals over the age of 65. This may explain its frequent inclusion in energy drinks and pre-workout formulations.
- Scientific Reports (2024) highlighted cognitive enhancements associated with taurine use.
Collectively, these studies suggest a broad and promising spectrum of health benefits associated with taurine supplementation.
However, it is critical to consider potential risks. A study published on May 14, 2025, in Nature, titled Taurine from Tumour Niche Drives Glycolysis to Promote Leukaemogenesis, reported that taurine may promote the growth of certain leukemia cell types. It is important to emphasize that this finding does not establish a causal link between taurine and cancer. Given that taurine is endogenously synthesized and essential for normal physiological function, its role in both healthy and pathological processes warrants nuanced interpretation.
It is plausible that, like many bioactive compounds, taurine may exert both beneficial and adverse effects depending on the context—supporting cellular function in healthy cells and potentially in malignant ones as well.
In conclusion, while the majority of commercial supplements offer minimal benefit and primarily profit manufacturers, taurine is supported by a growing body of data that justifies its use. Given its calming properties, a dosage of 2–3 grams taken at bedtime may be beneficial.
Please feel free to reach out with questions or comments.
Health Blog #11: Vitamins & Minerals–Do we need to take them?
By Jonathan A. Jarman, MD
Do You Need to Take Vitamins? The Answer: It Depends.
Approximately 1 in 3 Americans takes a multivitamin or multiple vitamin supplements daily.
According to the Centers for Disease Control and Prevention (CDC), the use of multiple dietary supplements increases with age. Among adults aged 60 and older, roughly 50% report taking more than one dietary supplement regularly.
In the United States, the vitamin and mineral retail market is projected to generate $3.06 billion in revenue by 2025. Globally, this market is estimated to reach $61.8 billion, underscoring the widespread reliance on supplementation.
Before addressing whether supplementation is necessary, it's helpful to understand the basic categories of vitamins.There are two primary types: water-soluble and fat-soluble vitamins.
This distinction is important because the body processes them differently.
- Water-soluble vitamins—which include vitamin C and the eight B vitamins—are not stored in significant amounts in the body. Excess quantities are typically excreted in the urine.
- Fat-soluble vitamins—vitamins A, D, E, and K—can accumulate in body tissues. Excessive intake may lead to toxicity, making these supplements riskier when consumed in high doses.
It’s also worth noting that the body can synthesize certain vitamins to a limited extent. These include vitamins D, K, B3 (niacin) and B7 (biotin).
While vitamin supplementation can be beneficial in some cases, it is not without risks. Whether or not one should take vitamins depends on diet, health condition and specific nutrient needs - all measurable via blood levels.
Summary Table of Vitamins the Body Can and Cannot Produce:

What Is the Evidence Supporting Vitamin Supplementation for Americans?
One of the most comprehensive studies on multivitamin use is the Physicians' Health Study II (PHS II), a large-scale, randomized, double-blind, placebo-controlled trial initiated in 1997 and concluded in 2011. Conducted by researchers at Brigham and Women’s Hospital and Harvard Medical School, the study involved 14,641 male physicians over the age of 50 who were administered a daily multivitamin (Centrum Silver) and followed for an average of 11.2 years.
While the PHS II is considered a well-designed and robust study, it has notable limitations. The study population was composed primarily of healthy, white, male physicians—a group that does not fully represent the diversity of the U.S. population. As a result, the generalizability of its findings to populations of different ages than the study cohort, women, individuals of other races or ethnicities and those with poor diets or chronic health conditions is limited.
Despite these constraints, the broader consensus remains: most Americans who consume a balanced diet are likely obtaining sufficient vitamins and minerals from food sources alone, and routine supplementation may offer little to no additional benefit. However, this does not mean that no one benefits from taking a multivitamin—individual needs and circumstances vary.
In 2022, the U.S. Preventive Services Task Force (USPSTF)—an independent, volunteer panel of national experts in disease prevention—published an Evidence Report analyzing 84 studies encompassing roughly 700,000 participants of both sexes. The task force found little to no evidence that vitamin and mineral supplements prevent early mortality, cancer, or cardiovascular disease—the leading causes of death in the United States. But the analysis only looked at disease prevention and not health optimization - an important distinction.
It is important to recognize the scope and perspective of the USPSTF. As a public health body, its recommendations are designed to inform care at the population level, often with a focus on cost-effectiveness. In short, they are not looking at the patient as an individual.
For instance, the same panel recommends against PSA (prostate-specific antigen) testing for prostate cancer screening in men over age 70. This guidance has been controversial; notably, President Biden’s prostate cancer was not diagnosed at an earlier stage because his physicians followed this recommendation.
In my view, such decisions—especially when it comes to individualized screening—are best made collaboratively by the patient and their physician, rather than being governed solely by national guidelines for groups with cost in mind.
What About Individuals with Inadequate Diets?
Data from the National Health and Nutrition Examination Survey (NHANES), conducted between 2003 and 2006 and reviewed by the CDC, indicate that although overall vitamin deficiency rates are relatively low in the U.S., certain demographic groups are disproportionately affected. These include individuals with limited access to nutritious food, certain racial and ethnic minorities, and people with specific health conditions.
In such cases, supplementation may be not only beneficial but necessary. Ultimately, the decision to take vitamin or mineral supplements should be informed by individual health status, dietary intake, and in some cases, medical testing—ideally under the guidance of a physician.
These deficient groups are:
Summary Table of Vitamin Deficiencies and Groups

Should You Take Vitamins? A Personalized Approach Beyond Population Guidelines
Thus far, the discussion has focused on population-level data regarding vitamin use. However, the decision to supplement should ultimately be individualized—based on the adequacy of one’s diet and, more precisely, one’s actual nutrient status as determined through laboratory testing.
Older Adults and Nutrient Deficiencies
Several studies suggest that older adults in the United States may particularly benefit from vitamin and mineral supplementation. This is due to age-related physiological changes that affect nutrient absorption, as well as dietary patterns that may lack essential micronutrients.
Common Nutrient Deficiencies in Older Adults
Data from the National Health and Nutrition Examination Survey (NHANES) conducted between 2003 and 2006. reveal substantial micronutrient inadequacies among U.S. adults aged 60 and older:
- Vitamin D: 95% have intakes below the Estimated Average Requirement (EAR)
- Vitamin E: 84% fall below the EAR
- Vitamin A: 45% have inadequate intake
- Vitamin C: 46% fall below the EAR
- Zinc: 15% have insufficient intake
These deficiencies can negatively impact immune function, bone integrity and cognitive performance. However, it is important to note that NHANES data reflect dietary intake, not measured vitamin levels, which introduces limitations in interpreting the prevalence and severity of true deficiencies.
I think it is very important to know that most vitamin and mineral testing recommendations from government and public health agencies (like the USPSTF, CDC, and IOM/NASEM) are focused primarily on avoiding disease and toxicity, not health optimization.
Evidence from Supplementation Studies
A 2012 study published in The Journal of Nutrition, Health & Aging titled “Vitamin Status in Elderly People in Relation to the Use of Nutritional Supplements” examined adults aged 70 to 90 and found:
- The status of vitamins A, C, and E was generally adequate.
- However, 88% had inadequate levels of vitamins D, K, and B6.
- Up to 10% were deficient in B1, B2, B12, and folate.
- Regular use of supplements significantly improved vitamin status.
The prevalence of poor nutritional status or malnutrition risk in older adults (>65 years) has been estimated to range between 4% and 25%. While supplementation can be beneficial, excessive intake of nutrients like iron and zinc—especially among older men—may lead to toxicity, highlighting the need for guided, evidence-based use.
Cognitive Health and Supplementation
Emerging research has linked certain nutrients to cognitive preservation and healthy aging:
- One study found that daily multivitamin use may help slow age-related cognitive decline.
- Another reported that vitamin D supplementation may protect telomere length, a marker of biological aging.
Given these findings, supplementation may be warranted for older adults in specific contexts:
- Vitamin D: Often needed due to reduced cutaneous synthesis with age.
- Vitamin B12: Absorption decreases with age; deficiency is linked to cognitive impairment.
- Calcium: Essential for bone health; may be needed if dietary intake is low.
- Magnesium and Zinc: Commonly deficient and crucial for many physiological processes.
Testing: Don’t Guess—Assess
To make informed decisions about supplementation, measuring your vitamin and mineral levels is key. Testing through a CLIA-certified laboratory, such as LabCorp, using advanced methods like LC-MS/MS (liquid chromatography–mass spectrometry), provides the most accurate results.
Most Commonly Tested Vitamins and Minerals


Conclusion
While most healthy adults in the U.S. with a balanced diet do not need routine vitamin or mineral supplementation, this changes with age.
Older adults are more likely to experience deficiencies due to changes in physiology and diet. Supplementation, when guided by clinical testing and physician oversight, can help maintain optimal health and prevent complications associated with nutrient deficits.
If you are concerned about your nutritional status, do not guess—ask your primary care physician to order appropriate vitamin and mineral tests. Personalized data provides the most reliable foundation for any decision regarding supplementation.
Health Blog #12: What is Heart Rate Variability (HRV) and why is it important?
Heart Rate Variability (HRV) is simply the variation in time between consecutive heartbeats. Specifically, it is the R–R interval period on an electrocardiogram (EKG).
HRV reflects the integration of brain, body and environment to include inflammation, recovery status, emotional regulation and even early neurodegeneration. As such many factors of health effect HRV. These factors will be addressed in this Longevity Tip.
While it might seem intuitive to think that the heart beats with perfect regularity—say, once every second if your heart rate is 60 bpm—the reality is more nuanced. Your heart may beat at 1.1 seconds, then 0.9 seconds, then 1.2 seconds and so on, BUT averaging out to 60 beats per minute.
These subtle fluctuations are not random noise—they carry profound physiological meaning and importance.
This is a diagram of HRV on an EKG strip.
The high spikes in the QRS electrical activity on an EKG are called the R tips. The average interval measurement period between EACH R tip is the Heart Rate Variability (HRV), usually measured over about 2.5 minutes in the morning.

Why HRV Matters
Contrary to popular belief, a consistent, clockwork heartbeat is not a sign of good health. In fact, more variability between beats—within a healthy range—indicates a more adaptable and resilient autonomic nervous system .
HRV Physiology in Simple Terms
I will try to make this as basic as possible to avoid putting anyone to sleep! You can skip this section if the way HRV works in our body is not of interest to you and move onto Influences of HRV.
In its most basic sense, HRV is controlled by the autonomic nervous system (ANS)—a branch of the peripheral nervous system (PNS) responsible for regulating involuntary functions like heart rate, breathing, and digestion.
The autonomic nervous system (ANS) is named for its "autonomous" or "self-governing" function — it operates largely unconsciously and automatically, without requiring voluntary control such as the higher central nervous system brain frontal lobes.
The term comes from:
- "Auto-" = self
- "Nomic" = governing (from the Greek nomos, meaning law or rule)
So the ANS governs bodily functions on its own — things like:
- Heart rate
- Blood pressure
- Respiration
- Digestion
- Pupil dilation/constriction
- Thermoregulation
- Sexual arousal
Even though it's unconscious, the ANS is tightly regulated by brain regions such as the hypothalamus, brainstem, and limbic system, and it can be indirectly influenced by your thoughts, emotions, and behavior (e.g., through breathwork or biofeedback training).
The ANS is composed of two main branches:
- Sympathetic Nervous System (SNS)
Classically called the “Fight or flight” part of the autonomic nervous system. The Sympathetic nervous system speeds up heart rate; primes body for action such as running from an animal that wants to eat you or getting into a fight on the playground. The SNS originates from the thoracic and lumbar spine. - Parasympathetic Nervous System (PNS)
Classically called the “Rest and digest” component of the ANS → Slows downheart rate; restores and conserves energy
Primarily mediated by the vagus nerve (cranial nerve X), which innervates the heart, lungs, GI tract, and more
These two systems constantly interact in a push-pull/yin yang dynamic.
For example:
When you inhale → vagal tone is inhibited by the SNS → HR increases slightly
When you exhale → vagal tone resumes → HR decreases slightly
This pattern is known as respiratory sinus arrhythmia, and it contributes directly to HRV.
Think of HRV as a real-time signal of your body's readiness:
- Athletes use HRV to guide training intensity.
- Doctors monitor HRV in ICU patients as a predictor of survival.
- Psychologists are exploring HRV biofeedback for anxiety and PTSD.
- Everyday users, like you and me, track HRV for insights into stress, sleep, and recovery.
In the early 2000s, HRV became measurable with wearables (e.g., Morpheus, Polar H10, Oura, WHOOP, Apple Watch, Elite HRV to name a few).
The most accurate wearables are those that use chest straps to directly measure your heart beats vs those that use a pulse to the skin on your wrist or finger.
I personally use the Morpheus Training System and Polar H10. The Morpheus for HRV guided cardio training/recovery and the Polar H10 to measure my HRV specifically in root mean square of successive differences (RMSSD). The Morpheus HRV combines a few parameters to provide their proprietary version of HRV and is NOT directly comparable to other system’s scores.
Hence, use the Morpheus for HRV guided recovery and training and not for an exact HRV score.
Influences of HRV
HRV is not a standalone measure of health, but it reflects key aspects of physiological status such as:
- Autonomic Nervous System Balance
- High HRV generally reflects a healthy dynamic between the sympathetic (“fight or flight”) and parasympathetic (“rest and digest”) branches of the autonomic nervous system (ANS).
- Low HRV may indicate sympathetic dominance, often seen with chronic stress, sleep disruption, overtraining, or illness.
2.Metabolic Health
- Obesity and insulin resistance lower vagal input and reduce HRV
3.Inflammation
- increased hsCRP and Il- 6, which we measure on all donors educes vagal tone and lowers HRV
- Physical Fitness and Cardiovascular Conditioning
- Athletes and physically fit individuals typically have higher resting HRV.
- As cardiovascular fitness improves, baseline HRV usually increases, reflecting enhanced parasympathetic tone and recovery capacity.
- Recovery and Readiness
- HRV is widely used in sports science to track recovery status and optimize training loads. I use it to plan my weekly cardio training routine.
- A drop in HRV can signal incomplete recovery, guiding athletes to adjust intensity or focus on rest.
- Stress and Sleep Quality
- Chronic psychological stress, emotional strain, and poor sleep all tend to suppress HRV.
- A consistently high HRV implies robust parasympathetic engagement and better coping capacity under stress.
- Alcohol (ETOH)
- Intake the night before measuring your HRV can reduce the score to less desirable.
- Ingestion the night before HRV morning measurement lowers HRV by boosting sympathetic activation, sleep disruption and inflammation.
- Drinking closer to 3-4 hours before sleep or increasing the dose of ETOH increases its negative effect on HRV.
- I encourage all who drink to measure their HRV in the morning after an evening of ETOH use, even if just a single drink.
- Resilience and System Flexibility
- HRV reflects how well your body adapts to internal and external stressors. It is a real-time biomarker of physiological resilience.
- Higher HRV is associated with greater adaptability and a healthier, more flexible nervous system.
- Long-Term Health Outcomes
- Low HRV is linked to increased risk of:
- Cardiovascular disease
- Type 2 diabetes
- Depression and anxiety
- All-cause mortality, especially post-myocardial infarction
- High HRV correlates with better cardiovascular health, emotional regulation, and longevity.
- Early Warning System
- Sudden drops in HRV can indicate:
- Overtraining
- Illness onset
- Poor sleep or excessive stress
- Lifestyle imbalances.
- Age
Age has a significant and well-documented impact on Heart Rate Variability (HRV): it tends to decrease with advancing age.
How Age Affects HRV
- General Trend
- HRV declines with agein both men and women.
- The parasympathetic branch (vagal tone)diminishes over time, while sympathetic activity often remains steady or becomes relatively more dominant.
- Early Adulthood to Middle Age
- In your 20s and 30s: HRV is generally at its highest.
- In your 40s–50s: There is a gradual decline, especially in high-frequency (HF) components that reflect parasympathetic activity.
- Older Adults (60s and beyond)
- HRV continues to decline more noticeably, with both time-domain and frequency-domain measures showing lower values.
- The autonomic nervous system becomes less flexible, reducing the body's ability to rapidly respond to stress or recover from exertion.
- Younger individualstypically have greater autonomic flexibility, enabling faster recovery and stronger stress resilience.
Aging-related decline in HRV has been associated with:
- Reduced baroreflex sensitivity
- Decreased vagal tone
- Slower recovery from stressors
- Increased risk of chronic disease
HRV Is Modifiable!
While aging affects HRV, it is not entirely fixed:
- Regular exercise (especially cardio aerobic and endurance)
- Good sleep hygiene
- Stress management (e.g., mindfulness, breathwork)
- Reduction of Metabolic Disease, e.g. obesity
- Minimized alcohol and stimulants
...can all help maintain or even improve HRV well into older age.
HRV by Age

Scientific Foundations
Awareness of HRV began in the early 20th century, but the landmark 1996 Task Force Report by the European Society of Cardiology and the North American Society of Pacing and Electrophysiology established formal standards for:
- HRV measurement (time-domain, frequency-domain, nonlinear methods)
- Physiological interpretation
- Clinical applications
This paper remains one of the most frequently cited references in HRV research.
In summary:
The fundamentals of HRV and why it is important.
- Indicator of Nervous System Balance
- High HRV → Strong parasympathetic activity (“rest and digest”), better adaptability.
- Low HRV → Sympathetic dominance (“fight or flight”), often linked to stress, fatigue, or illness.
- Stress and Recovery Monitor
- Tracks how well your body recovers from physical, emotional, or psychological stress.
- Helpful in guiding training intensity, workload, and rest days.
- Marker of Resilience and Adaptability
- Higher HRV is linked to greater physiological flexibility, meaning you can respond more effectively to challenges (physical or mental).
- Health and Longevity Correlations
- Low HRV is associated with increased risk of:
- Cardiovascular disease
- Diabetes
- Depression
- All-cause mortality (especially post-heart attack)
- High HRV is generally a sign of better cardiovascular health, fitness, and emotional regulation.
- Tool for Early Warning
- Sudden drops in HRV may signal:
- Overtraining
- Illness onset
- Poor sleep or high stress
- Imbalanced lifestyle choices
In a nutshell, HRV is a powerful biomarker of autonomic function, resilience, and overall system flexibility. Monitoring it can provide early insight into your physical and mental health, enabling proactive lifestyle adjustments for performance, longevity, and well-being.
Health Blog #13: Why Wearables Are Not the Answer for Fat Loss or Calorie Tracking
Why Wearables Are Not the Answer for Fat Loss or Calorie Tracking
By Jonathan A. Jarman, MD
(~ 4 minute read)
(~ 6 minute audio )
Exercise and diet are both fundamental parts of the health equation, but they play different roles. Diet is the primary driver of fat loss because it directly controls energy intake, while exercise supports health by improving metabolic fitness, preserving lean muscle, and boosting cardiovascular function. Yet, confusion often arises around how exercise fits into fat loss—and nothing has added more to this confusion than the devices on our wrists and gym equipment dashboards that spit out “calories burned.”
It seems simple enough. If our body fat is primarily driven by the calories we consume minus the calories we use in a day, then the formula is:
Calories Consumed in 24 hours – Calories Burned in 24 hours = Net Calories
So shouldn’t it be easy? Just eat fewer calories than you burn and the fat melts away, right? Yes—sort of. But not if you’re relying on what your Apple Watch, treadmill, or elliptical machine says about how many calories you’ve “torched.”
Here’s why. Imagine Bill, who eats 2000 calories per day as part of his Foundation’s health and fat-loss plan. His watch congratulates him: “Way to go, Bill! You just burned 500 calories in your squash match!” Bill now thinks he’s only at 1500 net calories for the day. That leads to two possible mistakes:
- He eats 500 extra calories as a reward because the watch told him he earned it.
- He doesn’t eat more, but he walks around thinking he’s created a huge deficit when in reality, the device’s estimate may be way off.
This is the trap: we take inaccurate calorie burn numbers as truth, and it shapes our choices in ways that sabotage our goals.
The Problem With Calorie Estimates
Research has consistently shown that wearable calorie estimates are unreliable. A 2017 Stanford study on seven popular devices found that while heart rate measurements were fairly accurate (average error ~5%), calorie burn estimates were off by an average of 27%, and sometimes by as much as 93% (Shcherbina et al., 2017).
Fast forward to a 2025 University of Mississippi study on the Apple Watch Series 9: the device’s average error for calorie burn was 27.96%, across walking, running, cycling, and mixed workouts (University of Mississippi, 2025).
And it’s not just Apple. A 2024 umbrella review confirmed that across multiple brands, calorie burn estimates often deviated by ±20% or more—making them far from precise tools (Ding et al., 2024).
Why Devices Get It Wrong
Wearables rely on accelerometers, optical heart rate sensors, and algorithms. But calorie burn depends on far more than wrist motion and heart rate. Age, sex, body composition, metabolic efficiency, and even skin tone can alter results.
For example:
- Resistance training and cycling often produce huge errors because there’s little wrist movement.
- Skin pigmentation or tattoos can interfere with optical sensors, reducing accuracy (O’Driscoll et al., 2024).
In short: the watch doesn’t know you—your metabolism, your efficiency, your unique biology. It just guesses.
The Real Fat Loss Equation
At the end of the day, fat loss comes from a consistent calorie deficit. But you don’t need precise burn numbers from a device to achieve this. In fact, relying on those numbers can backfire:
- People overestimate exercise calories, then eat more (“I earned dessert”).
- Devices ignore non-exercise activity (walking, chores, fidgeting), which often contributes more to daily burn than a single workout.
- Chasing false precision distracts from building sustainable habits.
Think of it this way: diet controls intake and directly drives fat loss, while exercise supports the process by improving health, strength, and performance. They complement each other, but they’re not interchangeable.
Smarter Alternatives
If calorie burn estimates are so flawed, what should you focus on instead?
- Use wearables for heart rate, HRV and step tracking, where they’re far more reliable.
- Watch trends in body weight over weeks, not day-to-day fluctuations.
- Measure waist circumference, strength gains, or progress photos as signs of change.
- Pay attention to nutrition tracking, since intake is easier to measure than expenditure.
The Takeaway
Wearables are fantastic for motivation, accountability, and activity reminders. But when it comes to fat loss, they’re not trustworthy calorie accountants. Science shows they routinely miss the mark—sometimes by 20–40%, sometimes by much more. Instead of chasing misleading numbers, focus on the fundamentals: eat well, move consistently, train with purpose, and track progress with tools that matter.
References
- Shcherbina, A. et al. (2017). Accuracy in wrist-worn, sensor-based measurements of heart rate and energy expenditure in a diverse cohort. Journal of Personalized Medicine. Stanford Medicine
- University of Mississippi (2025). Apple Watch accuracy study. Ole Miss News
- Ding, D. et al. (2024). Accuracy of wearable devices in estimating energy expenditure: umbrella review. Sports Medicine. Springer
- O’Driscoll, R. et al. (2024). Variations in accuracy of Apple Watch energy expenditure estimates by skin pigmentation. Sports, 12(4), 275. MDPI
Health Blog #14: Can Better Cardio Help Us Make Muscle? - 10.10.25
Longevity Tip 7
Can Better Cardio Help Us Make Muscle?
By Jonathan A. Jarman MD
(~3 min read)
(~4 min audio)
No way, right? Runners are skinny, have low bone density and are not strong. Right? True. Runners are prone to injury due to lack of bone density and strength. Right? True.
Trying to get a runner to do resistance training is like asking someone who only runs marathons to try a pull-up. Can’t happen.
So then if all this is true – and it is – how can cardio training, and a better VO₂Max that comes with it, help build muscle?
As my cardio and measured VO₂Max improved from playing tennis 5–7 times a week and completing my Morpheus weekly cardio goals, I noticed I was less fatigued between resistance training sets. I did research to see if what I noticed had a body of scientific evidence.
It does.
This blog is written with those of you in mind who hate cardio but love resistance training. If you want optimum health, you have to be focused on both.
Cardio training is essential for VO₂Max and numerous studies confirm VO₂Max is the single most important metric for longevity. Yet VO₂Max is not related to a strong body. (1,2,3,4,5)
First, know that resistance training does NOT contribute to cardio Zone training. I have found a lot of confusion with resistance training HR and Cardio Zones. Even if you are in Zone 2 during resistance training, it does NOT contribute to your weekly cardio zone training needs. No need to think about your heart rate while pumping iron.
And yet the opposite is true and that’s the gist of this blog. Improved VO₂Max (cardiorespiratory fitness) does improve resistance-training sets without loss of performance.
For those of you who don’t enjoy cardio training, this is how it will benefit your resistance training gains. It will make your muscle building workouts more efficient.
As your VO₂Max improves, your needed rest time between sets will reduce.
We have to rest between resistance sets because we use up stored muscle energy (ATP and phosphocreatine (PCr)) during lifting and have to allow the body to replace these molecules during rest.
After depletion from lifting, PCr resynthesis requires oxygen and mitochondrial activity, taking roughly 2–5 minutes to restore fully. Also, moderate- to high-rep sets accumulate lactate and H⁺ ions, lowering muscle pH. As you know, I am not a fan of high-rep sets for building power. Low-rep sets at higher weight build power.
Rest allows time for lactate clearance and buffering, so contractile performance recovers.
Shorter rest means incomplete PCr recovery → lower force and power output in the next set. This IS important. You need full recovery to recruit your muscle building forces to maximally build muscle and power.
There is also central (brain) and peripheral nerve issues with lifting as heavy lifting involves high motor unit recruitment and central nervous system drive.
Rest periods let the nervous system re-prime for maximal output — especially important for compound lifts or near-maximal loads. Note that older lifters benefit from slightly longer rest for neural recovery — but improved aerobic capacity can offset some of that.
Optimal rest varies based on goals. (6)

This is the crux for how cardio fitness helps resistance training fitness. Higher VO₂max → faster PCr and lactate recovery plus ATP replenishment → you can trim rest intervals by 20–50% while keeping output stable.(7)
So, if you improve your cardio, you will rest less between sets and get MORE done in the same amount of time. You will accumulate greater total training volume per session.
In summary, increasing VO₂max improves cardiovascular and metabolic recovery between sets, enabling shorter rest without fatigue buildup. This enhances training efficiency and total work output — one of the reasons elite athletes across sports (including power and team sports) prioritize aerobic capacity alongside strength.
VO₂max builds your engine. Strength builds your chassis. You want both if your goal is performance and longevity.
References
- Kodama S, et al. Cardiorespiratory fitness as a quantitative predictor of all-cause mortality and cardiovascular events: a meta-analysis. JAMA 2009. (1-MET ≈ 13% lower all-cause mortality). JAMA Network
- Mandsager K., et al. Association of Cardiorespiratory Fitness With Long-term Mortality Among Adults Undergoing Exercise Treadmill Testing. JAMA Netw Open 2018. (122,007 patients; elite vs low HR 0.20). JAMA Network
- Ross R., et al. Importance of Assessing Cardiorespiratory Fitness in Clinical Practice: A Case for Fitness as a Clinical Vital Sign. AHA Scientific Statement, Circulation 2016. PubMed
- Lang JJ., et al. Cardiorespiratory fitness is a strong and consistent predictor of risk across many mortality outcomes — overview 2024. (Systematic-review-of-reviews). PMC
- Milanović Z., et al. Endurance vs HIIT for VO₂max — systematic review & meta-analysis. 2015 (and subsequent HIIT meta-analyses) — show VO₂max is trainable; HIIT often superior or similar. PubMed+1
- . Bogdanis, G. C., Nevill, M. E., Boobis, L. H., Lakomy, H. K. A., & Nevill, A. M. (1996). Recovery of power output and muscle metabolites following 30 s of maximal sprint cycling in man. Journal of Applied Physiology, 80(3), 876–884. https://doi.org/10.1152/jappl.1996.80.3.876
- Tomlin, D. L., & Wenger, H. A. (2001). The relationship between aerobic fitness and recovery from high intensity intermittent exercise. Sports Medicine, 31(1), 1–11. https://doi.org/10.2165/00007256-200131010-00001
Health Blog #17: How to evaluate health care advice in the media and internet.
Ut tempor et magna ut Lorem ut et. Elit eiusmod ipsum amet incididunt eiusmod et. Sed eiusmod sit aliqua. Magna sed Lorem dolore do dolor. Consectetur sit labore labore consectetur ipsum.
Labore adipiscing aliqua. Lorem eiusmod magna eiusmod. Amet consectetur amet sed elit ut et tempor. Dolor consectetur aliqua. Dolore elit sed dolore. Ut ipsum aliqua. Labore magna dolor adipiscing amet. Aliqua aliqua dolore eiusmod sed aliqua.
Amet aliqua ipsum sit. Consectetur tempor consectetur sit. Lorem ut elit dolor. Consectetur eiusmod tempor dolore. Et sit aliqua. Aliqua tempor.
Elit consectetur incididunt tempor sed ut sed. Dolore dolore ipsum ut et ipsum. Eiusmod incididunt dolor tempor adipiscing aliqua. Magna incididunt. Magna sit Lorem magna dolore dolore consectetur ipsum. Magna consectetur ipsum ipsum Lorem.
Dolore do sit ut elit magna. Do do incididunt aliqua. Aliqua magna et incididunt. Adipiscing dolor adipiscing et. Incididunt Lorem labore sit. Consectetur ut labore tempor ut sed aliqua.
Health Blog #18: Cognitive improvement with supplements - can jelly fish make us smarter?
Ut tempor et magna ut Lorem ut et. Elit eiusmod ipsum amet incididunt eiusmod et. Sed eiusmod sit aliqua. Magna sed Lorem dolore do dolor. Consectetur sit labore labore consectetur ipsum.
Labore adipiscing aliqua. Lorem eiusmod magna eiusmod. Amet consectetur amet sed elit ut et tempor. Dolor consectetur aliqua. Dolore elit sed dolore. Ut ipsum aliqua. Labore magna dolor adipiscing amet. Aliqua aliqua dolore eiusmod sed aliqua.
Amet aliqua ipsum sit. Consectetur tempor consectetur sit. Lorem ut elit dolor. Consectetur eiusmod tempor dolore. Et sit aliqua. Aliqua tempor.
Elit consectetur incididunt tempor sed ut sed. Dolore dolore ipsum ut et ipsum. Eiusmod incididunt dolor tempor adipiscing aliqua. Magna incididunt. Magna sit Lorem magna dolore dolore consectetur ipsum. Magna consectetur ipsum ipsum Lorem.
Dolore do sit ut elit magna. Do do incididunt aliqua. Aliqua magna et incididunt. Adipiscing dolor adipiscing et. Incididunt Lorem labore sit. Consectetur ut labore tempor ut sed aliqua.
Health Blog #19 - Health After 40: Why Muscle & VO₂max Predict Longevity Better Than Lab Tests
An evidence-based review
Jonathan A. Jarman, MD is a Yale–NYU trained physician engaged in health-optimization and longevity research. His work focuses on the physiology of high-performance aging, including VO₂max, muscle strength, autonomic regulation, emotional control, and cognitive resilience. He leads the Julian A. Jarman MD Research Foundation, which supports and advances research in these domains.
I entered my mid-60s and was suddenly facing multiple medical diagnoses across several organ systems. None were individually catastrophic. Taken together, however, they pointed toward a trajectory I did not like and were already eroding my quality of life. My mortality felt closer than I was willing to accept.
That realization was a wake-up call—and I chose to answer it.
Doing so required a complete reset of how I thought about my own health and behavior—neither of which aligned with building an optimal body—as well as a fundamental reconsideration of Western medicine itself. This was not a so-called midlife crisis. I was in my 60s, medically unwell, and became engaged in a disciplined, evidence-based effort to define optimal health—and earn my way back to it.
I should be clear: I received no formal training in any of this during medical school or residency. That statement is not a criticism; it is an observation. Our medical system—including the board examinations every physician must pass—is designed to diagnose and treat disease, not to define, measure, or build high-level health.
We are taught how to manage heart failure, but not how to prevent the physiologic decline that precedes it. We learn how to interpret troponins and lipid panels, but not why VO₂max and skeletal muscle mass predict mortality more strongly than many routinely targeted laboratory markers.
Most people have seen a VO₂max test on television in elite athletes—typically performed on a bike or treadmill, with a tight mask sealed over the nose and mouth and tubing connected to a metabolic cart. VO₂max measures cardiorespiratory fitness, specifically the maximum amount of oxygen the body can utilize during intense exercise.
In simple terms: VO₂max is a direct measure of how well the heart, lungs, blood, muscles, and mitochondria work together under stress. The higher the VO₂max, the greater the physiologic capacity—and the lower the risk of premature mortality.
With this mind set, rather than simply “treat my disease” with surgery and medication, I spent the next year researching what it truly means to build optimum health from the ground up. My goal was not merely to manage decline through traditional medicine, but to reverse disease burden and optimize my physiology for longevity and quality of life.
If most physicians do not understand this relationship, it is because none of us were trained to.
I had to learn it later—through a year of research, training, self-experimentation, and immersion in the longevity science literature.
What Changed When I Stopped Managing Disease and Started Building Capacity
During that year of research, training, and experimentation, I lost roughly 40 pounds of fat—not weight, but fat—and gained more than 15 pounds of skeletal muscle. This transformation aligns with decades of research demonstrating that older adults can reliably gain muscle and lose fat with structured resistance training and adequate protein intake⁽¹⁾.
By the end of the year, at age 65, I bench-pressed 275 pounds. I will share this on video—not as a stunt, but as a demonstration that meaningful physiologic adaptation remains possible well into later decades of life.
Many people assume that building muscle later in life is “too hard,” “too dangerous,” “unnecessary,” “vanity-driven,” or “not for women.” This belief is not merely incorrect—it is actively harmful.
The evidence is unequivocal: older adults can gain muscle and strength and often do so more safely than younger adults when training is properly supervised and structured⁽²⁵,³⁵–³⁹⁾. The real danger is not training. It is avoiding the single intervention that most reliably protects independence, metabolic health, and longevity⁽¹⁴,¹⁵,³⁶⁾.
The hardest task for any physician is not prescribing another medication or explaining why the latest supplement dominating social media is ineffective—despite the relentless promotion of snake-oil solutions online—but convincing patients that sustained behavioral change remains the most powerful intervention available.
This is something I experience repeatedly at the Foundation.
Muscle and aerobic capacity are built, not prescribed.
They cannot be ordered.
They must be earned.
Yet they predict long-term health, functional independence, and survival more strongly than many commonly targeted laboratory markers and single-pathway pharmacologic interventions⁽³⁷–⁴⁰⁾.
VO₂max: Where the Argument Becomes Unavoidable
With strength rebuilt and total body fat about 23%, the next frontier was cardiorespiratory fitness and VO₂max—one of the strongest predictors of cardiovascular and all-cause mortality across populations⁽²⁾.
Before beginning focused aerobic training, my echocardiogram showed Grade I diastolic dysfunction, a common and often reversible finding with aging⁽³⁾. At that time, my VO₂max was approximately 28, considered “fair” for my age.
I initially built my aerobic base with Zone 2 jogging, then transitioned to tennis as my primary aerobic modality. To guide recovery and avoid overtraining, I incorporated daily heart rate variability (HRV) monitoring using the Morpheus system⁽⁴⁾.
HRV-guided feedback was used to adjust training intensity across the week, allowing confirmation that aerobic workload targets were being met.
In practice, I found it easier to achieve all of my target training zones through tennis than through jogging.
Within just a few months of playing tennis 5–6 times per week for 1–2 hours per session, my VO₂max increased to 34—considered good to excellent—and associated
with substantially lower mortality risk⁽²⁾. A repeat echocardiogram showed complete resolution of diastolic dysfunction⁽⁵⁾.
At this point, the physiology becomes difficult to ignore.
Large population studies consistently show higher VO₂max is strongly associated with lower cardiovascular and all-cause mortality. Because VO₂max integrates cardiac, pulmonary, muscular, neurologic, and metabolic function, it reflects whole-body physiologic capacity, rather than the performance of any single organ.
What follows is practical: VO₂max should be trained, measured, and treated as one of the primary health metrics for many—not a secondary fitness curiosity.
Subjectively, the difference is dramatic. I can play tennis for hours against people half my age, sustain heart rates in the mid-140s, and feel completely fine. This reflects improved VO₂max and enhanced whole-body aerobic performance⁽⁶⁾.
The combination of global longitudinal strain (GLS) on echocardiography and direct VO₂max testing provides one of the most accurate assessments of cardiac performance and systemic oxygen utilization⁽⁷⁾.
This personal transformation ultimately inspired the creation of the Julian A. Jarman, MD Research Foundation, Inc., with the goal of better understanding how the practice of medicine can optimize—not merely manage—health.
Is it false to say that if a man in his mid-60s can do this, everyone can? Technically, yes. But it is overwhelmingly true, in the absence of advanced disease, that the majority of people who believe they “can’t” are limited not by age or biology, but by low expectations, lack of knowledge, and the absence of proper training.
The Distraction Problem
Patients, friends, and social media followers are constantly searching for a “Fountain of Youth” in supplements, medications, and laboratory tests. The irony is that this relentless pursuit of shortcuts actively distracts from the only interventions that consistently and reproducibly work.
Social media has amplified this problem. Much of what is marketed as “health” content is misleading or false—and it trains people to chase noise instead of building physiologic capacity.
The purpose of this blog is to redirect attention away from that noise and toward what actually determines long-term health, functional independence, and survival.
The framework presented here is not what U.S. medicine currently offers to most patients, and for many it will create cognitive dissonance. That is intentional. The prevailing U.S. medical model is designed to diagnose and manage disease—not to define, measure, or build health optimization.
For that reason, every position in this blog is grounded in rigorous scientific evidence—not opinion, ideology, or anecdote. This represents a necessary paradigm shift, driven by decades of outcomes-based research showing that cardiorespiratory fitness and skeletal muscle capacity outperform traditional risk markers in predicting long-term health and survival⁽²,⁸,²⁴,²⁶,³⁴,³⁷–³⁹,⁴⁸–⁵¹⁾.
This blog is not a criticism of the treatment of disease with medication or surgery. Rather, it highlights a complementary path—one that is rarely addressed in most U.S. medical offices—focused on building and preserving physiologic capacity to optimize health and achieve the greatest possible longevity.
This blog is about the real “Fountain of Youth.”
What Most People Get Wrong About Health After 40
The internet is filled with misleading or outright false statements about aging, exercise, and what is “safe” or “possible” after 40. If it’s on social media, it is probably wrong—and often designed to sell you something of unproven value.
These myths don’t just confuse people; they cause real harm by lowering expectations, discouraging training intensity, and convincing older adults that decline is inevitable.
Below are two of the most common misconceptions—and the evidence-based corrections.
Myth #1 — “Walking or any movement is good enough.”
Walking is healthy.
But walking alone is rarely sufficient to meaningfully raise VO₂max or preserve skeletal muscle mass with aging.
Step counts and activity rings track movement, not physiologic adaptation. If movement does not impose sufficient intensity or progressive overload, it will not meaningfully improve VO₂max, strength, or long-term health.
VO₂max improves through adequate intensity—most often sustained Zone 2 training… layered with periodic higher-intensity efforts.
Walking is beneficial for mood, joint health, and general well-being—but it is not, by itself, a comprehensive training strategy for preserving physiologic capacity after midlife.
Myth #2 — “Building muscle after 40 is too dangerous.”
False.
Older adults can gain muscle reliably and safely under structured training programs⁽³⁵–³⁹⁾. In many cases, they do so with lower injury rates than younger individuals when programs are appropriately designed and supervised.
The greater danger is the opposite:
Avoiding strength training → frailty → falls → hospitalization → accelerated decline. Strength training is not reckless.
It functions as protective medicine.
Myth #3 — “When my heart rate increases during resistance training, that time counts toward my cardio zone training.”
This is a common and understandable misconception. It is intuitive to think that if heart rate rises during any form of exercise, it must contribute to cardiovascular fitness—since cardiovascular training also requires an elevated heart rate.
But this is incorrect.
Resistance training can raise heart rate—but heart rate elevation alone does not define cardiovascular training, nor does it improve VO₂max in a meaningful way.
Why?
• VO₂max improves through sustained, rhythmic, aerobic demand, where large muscle groups continuously consume oxygen over time
• Resistance training is intermittent by design, consisting of short bursts of effort followed by rest
• During lifting, heart rate rises primarily due to pressure responses, bracing, and sympathetic activation, not sustained oxygen utilization.
• The cardiovascular system is never stressed long enough to trigger the structural adaptations required for VO₂max improvement (e.g., increased stroke volume, capillary density, mitochondrial biogenesis)
In simple terms:
• Lifting trains force production
• Cardio trains oxygen delivery and utilization
• A fast pulse during lifting reflects acute stress, not aerobic conditioning
This distinction matters clinically.
Time spent lifting—even when heart rate is elevated—does not accumulate toward cardio “zone time”, and it does not substitute for deliberate aerobic training. Both systems are essential, but they adapt through fundamentally different mechanisms.
This is why muscle and VO₂max must be trained separately—and intentionally to optimize health.
Hormone Optimization: The Often-Ignored Prerequisite for Training After 50
One reality rarely discussed—yet consistently supported in research—is that many adults over 50 cannot build muscle or improve aerobic capacity effectively without first correcting hormonal deficiencies.
Testosterone and estrogen decline with age, directly impairing:
- Muscle protein synthesis
- Recovery capacity
- Mitochondrial function
- Aerobic performance
- Motivation, drive, and energy
These aren’t “soft symptoms.”
They are measurable physiologic barriers.
This leads to one of the most damaging myths:
“I can’t lift heavy or train intensely because I’m old.”
In reality, many people can’t train intensely because their hormones are too low to support adaptation—not because of age itself.
When supervised appropriately, hormone replacement can help restore the physiologic environment required for:
- Strength training
- Muscle hypertrophy
- VO₂max improvement
- Recovery capacity
- Consistency
HRT does not replace training.
It enables it.
For many women over 50 and many men over 60, HRT is not optional—it is the physiologic prerequisite for meaningful strength and VO₂max adaptation.
If You’re Over 40, You’ve Probably Noticed Something Important
No one is coming to save your health for you.
Your doctor can monitor it—but most are not trained in building or optimizing long-term health.
Your lab work can reflect it.
Your medications can support it.
No modifiable factor protects your health as powerfully as:
- Muscle
- Aerobic fitness (VO₂max)
Both are independently associated with⁽²,⁸⁾:
- Lower all-cause mortality
- Lower cardiovascular risk
- Greater independence
- Better metabolic and brain health
Despite the widespread reliance on laboratory testing to assess health, muscle strength and aerobic fitness (VO₂max) are among the strongest independent predictors of survival ever identified—often outperforming traditional laboratory markers and cardiovascular risk factors.⁽²,⁸⁾
At the Foundation, muscle and VO₂max are the primary determinants of functional longevity—how well you live, not just how long.
Why VO₂max Outperforms Nearly Every Laboratory Marker
Modern medicine indeed places heavy emphasis on blood tests as indicators of health. While these measures are often clinically valuable, most laboratory tests reflect isolated pathways or individual organ systems, not whole-body physiologic capacity.
Metrics such as VO₂max dixer precisely because they require coordinated performance across nearly every major organ system.
To achieve even an average VO₂max, nearly every major organ system must be functioning well, including:
- Cardiovascular system
- Pulmonary system
- Hematologic system
- Musculoskeletal system
- Central and peripheral nervous systems
- Endocrine system
- Renal and hepatic systems
In practice, VO₂max functions as a whole-organism stress test.
If any major system is impaired, VO₂max declines.
This is why VO₂max is so powerfully predictive of survival—and why improving VO₂max often normalizes many laboratory abnormalities, rather than the other way around. This relationship is frequently misunderstood in clinical practice, leading to misplaced priorities in care.
If we have decades of data demonstrating the importance of VO₂max, DEXA-derived body composition, and the preservation of muscle mass for long-term health, a reasonable question follows: why has Western medicine not adopted these measurements—or organized care around what they so clearly predict?
That question matters. The answer is complex, involving structural, cultural, and economic forces. It deserves its own discussion—and lies beyond the scope of this article. It may be addressed in a future piece.
Muscle: The Central Organ of Independence
For those who believe muscle is unimportant or “just vanity,” this must be stated clearly:
Muscle is not just cosmetic.
It is structural, metabolic, and protective.
Why muscle matters after 40, 50, 60, 70, 80, and beyond:
- Improves balance and stability, reducing fall risk⁽⁹⁾
- Preserves mobility and daily function⁽¹⁰⁾
- Stimulates bone remodeling and skeletal integrity⁽¹¹⁾
- Enhances insulin sensitivity and glucose disposal⁽¹²⁾
- Raises resting metabolic rate and metabolic flexibility⁽¹³⁾
- Provides physiologic reserve during illness, injury, or surgery⁽¹⁴⁾
Tendon Health (An Often-Overlooked—and Often Misunderstood—Benefit of Strength Training)
Tendons are living tissue that adapt—slowly—to mechanical loading. With aging and inactivity, they stiffen, thin, lose collagen quality, and become more injury-prone.
Paradoxically, many people believe resistance training should be avoided with age to ‘protect’ tendons. The opposite is true: it is under-loading—not progressive, appropriately dosed loading—that accelerates tendon degeneration. Properly programmed strength training preserves not just muscle, but the muscle–tendon unit, which is essential for force transmission, joint stability, and injury prevention. ⁽¹⁵,¹⁶⁾
Key tendon-specific benefits of resistance training
- Preserves tendon stiffness and elasticity, improving force transfer and movement efficiency⁽¹⁵⁾
- Reduces the risk of tendon rupture and overuse injury, particularly in the Achilles, patellar, and rotator cuff tendons⁽¹⁶⁾
- Improves rate of force development, critical for balance recovery and fall prevention⁽¹⁷⁾
- Maintains joint stability under load, reducing compensatory movement and arthritis progression⁽¹⁸⁾
- Supports power and deceleration—not just strength—essential for stair climbing, rising from chairs, and fall prevention⁽¹⁹⁾
Like VO₂max, muscle represents physiologic capacity.
Within physiologic limits, there is no upper “normal” threshold—greater capacity confers greater resilience.
Muscle Metrics We Track at the Foundation
Grip strength, commonly used in research and some medical practices, is simple and predictive at a population level. However, for individuals over 40, we think it poorly captures the traits that most strongly determine independence and real-world function.
At the Foundation, we therefore favor age- and sex-normalized, whole-body functional strength measures that better reflect true physiologic capacity.
Foundation Functional Strength Index (FSI)
We begin with DEXA-derived appendicular lean mass (ALM), indexed to height².
DEXA scan derived ALM/ht² is one of the most extensively validated measures of skeletal muscle mass and has been used for over two decades to define sarcopenia and predict disability, frailty, and mortality⁽⁴¹–⁴⁴⁾.
Major international consensus groups—including the European Working Group on Sarcopenia in Older People (EWGSOP2) and Asian Working Group for Sarcopenia (AWGS)—recognize DXA scan measured ALM/ht² as a standard method for quantifying muscle mass in aging populations⁽⁴⁵–⁴⁷⁾.
BMI and scale weight provide little insight into aging physiology. In contrast, ALM/ht² directly measures skeletal muscle, making it vastly superior for assessing frailty risk, functional capacity, and long-term health outcomes.
Physiologic Capacity: Performance Contextualization
Physiologic capacity is best interpreted in context. Individual performance is therefore evaluated relative to age- and sex-specific normative distributions derived from large population datasets.
Percentile rankings for aerobic fitness (VO₂max) are based on established normative tables from the Cooper Institute and are referenced by the American College of Sports Medicine (ACSM)⁽⁴⁸⁾. Additional population-level reference values are available from large national datasets, including Canadian health surveys, which report age- and sex-specific percentiles for cardiorespiratory fitness⁽⁴⁹⁾. Together, these sources allow aerobic capacity to be meaningfully contextualized relative to demographic peers.
To complement DEXA-derived appendicular lean mass (ALM), we incorporate a three-movement functional strength battery assessing whole-body force production and transfer:
- Push-ups — upper-body and trunk strength
- Air squats — lower-body strength, coordination, and power
- Knee-bent, unanchored sit-ups — trunk endurance and force transmission
We use knee-bent, unanchored sit-ups rather than curl-ups because they assess functional trunk strength through a full range of motion that more closely reflects real-world tasks, including rising from the floor and maintaining independence with aging. Variants of this test have also been used for decades by the U.S. military as a practical, scalable measure of trunk strength and conditioning.
Performance Targets After 40
- Minimum target: ≥75th percentile for age and sex
- Ideal Foundation goal: ≥90th percentile
- See FSI Bands below to understand where you sit

An evidence-based review
Jonathan A. Jarman, MD is a Yale–NYU trained physician engaged in health-optimization and longevity research. His work focuses on the physiology of high-performance aging, including VO₂max, muscle strength, autonomic regulation, emotional control, and cognitive resilience. He leads the Julian A. Jarman MD Research Foundation, which supports and advances research in these domains.
I entered my mid-60s and was suddenly facing multiple medical diagnoses across several organ systems. None were individually catastrophic. Taken together, however, they pointed toward a trajectory I did not like and were already eroding my quality of life. My mortality felt closer than I was willing to accept.
That realization was a wake-up call—and I chose to answer it.
Doing so required a complete reset of how I thought about my own health and behavior—neither of which aligned with building an optimal body—as well as a fundamental reconsideration of Western medicine itself. This was not a so-called midlife crisis. I was in my 60s, medically unwell, and became engaged in a disciplined, evidence-based effort to define optimal health—and earn my way back to it.
I should be clear: I received no formal training in any of this during medical school or residency. That statement is not a criticism; it is an observation. Our medical system—including the board examinations every physician must pass—is designed to diagnose and treat disease, not to define, measure, or build high-level health.
We are taught how to manage heart failure, but not how to prevent the physiologic decline that precedes it. We learn how to interpret troponins and lipid panels, but not why VO₂max and skeletal muscle mass predict mortality more strongly than many routinely targeted laboratory markers.
Most people have seen a VO₂max test on television in elite athletes—typically performed on a bike or treadmill, with a tight mask sealed over the nose and mouth and tubing connected to a metabolic cart. VO₂max measures cardiorespiratory fitness, specifically the maximum amount of oxygen the body can utilize during intense exercise.
In simple terms: VO₂max is a direct measure of how well the heart, lungs, blood, muscles, and mitochondria work together under stress. The higher the VO₂max, the greater the physiologic capacity—and the lower the risk of premature mortality.
With this mind set, rather than simply “treat my disease” with surgery and medication, I spent the next year researching what it truly means to build optimum health from the ground up. My goal was not merely to manage decline through traditional medicine, but to reverse disease burden and optimize my physiology for longevity and quality of life.
If most physicians do not understand this relationship, it is because none of us were trained to.
I had to learn it later—through a year of research, training, self-experimentation, and immersion in the longevity science literature.
What Changed When I Stopped Managing Disease and Started Building Capacity
During that year of research, training, and experimentation, I lost roughly 40 pounds of fat—not weight, but fat—and gained more than 15 pounds of skeletal muscle. This transformation aligns with decades of research demonstrating that older adults can reliably gain muscle and lose fat with structured resistance training and adequate protein intake⁽¹⁾.
By the end of the year, at age 65, I bench-pressed 275 pounds. I will share this on video—not as a stunt, but as a demonstration that meaningful physiologic adaptation remains possible well into later decades of life.
Many people assume that building muscle later in life is “too hard,” “too dangerous,” “unnecessary,” “vanity-driven,” or “not for women.” This belief is not merely incorrect—it is actively harmful.
The evidence is unequivocal: older adults can gain muscle and strength and often do so more safely than younger adults when training is properly supervised and structured⁽²⁵,³⁵–³⁹⁾. The real danger is not training. It is avoiding the single intervention that most reliably protects independence, metabolic health, and longevity⁽¹⁴,¹⁵,³⁶⁾.
The hardest task for any physician is not prescribing another medication or explaining why the latest supplement dominating social media is ineffective—despite the relentless promotion of snake-oil solutions online—but convincing patients that sustained behavioral change remains the most powerful intervention available.
This is something I experience repeatedly at the Foundation.
Muscle and aerobic capacity are built, not prescribed.
They cannot be ordered.
They must be earned.
Yet they predict long-term health, functional independence, and survival more strongly than many commonly targeted laboratory markers and single-pathway pharmacologic interventions⁽³⁷–⁴⁰⁾.
VO₂max: Where the Argument Becomes Unavoidable
With strength rebuilt and total body fat about 23%, the next frontier was cardiorespiratory fitness and VO₂max—one of the strongest predictors of cardiovascular and all-cause mortality across populations⁽²⁾.
Before beginning focused aerobic training, my echocardiogram showed Grade I diastolic dysfunction, a common and often reversible finding with aging⁽³⁾. At that time, my VO₂max was approximately 28, considered “fair” for my age.
I initially built my aerobic base with Zone 2 jogging, then transitioned to tennis as my primary aerobic modality. To guide recovery and avoid overtraining, I incorporated daily heart rate variability (HRV) monitoring using the Morpheus system⁽⁴⁾.
HRV-guided feedback was used to adjust training intensity across the week, allowing confirmation that aerobic workload targets were being met.
In practice, I found it easier to achieve all of my target training zones through tennis than through jogging.
Within just a few months of playing tennis 5–6 times per week for 1–2 hours per session, my VO₂max increased to 34—considered good to excellent—and associated
with substantially lower mortality risk⁽²⁾. A repeat echocardiogram showed complete resolution of diastolic dysfunction⁽⁵⁾.
At this point, the physiology becomes difficult to ignore.
Large population studies consistently show higher VO₂max is strongly associated with lower cardiovascular and all-cause mortality. Because VO₂max integrates cardiac, pulmonary, muscular, neurologic, and metabolic function, it reflects whole-body physiologic capacity, rather than the performance of any single organ.
What follows is practical: VO₂max should be trained, measured, and treated as one of the primary health metrics for many—not a secondary fitness curiosity.
Subjectively, the difference is dramatic. I can play tennis for hours against people half my age, sustain heart rates in the mid-140s, and feel completely fine. This reflects improved VO₂max and enhanced whole-body aerobic performance⁽⁶⁾.
The combination of global longitudinal strain (GLS) on echocardiography and direct VO₂max testing provides one of the most accurate assessments of cardiac performance and systemic oxygen utilization⁽⁷⁾.
This personal transformation ultimately inspired the creation of the Julian A. Jarman, MD Research Foundation, Inc., with the goal of better understanding how the practice of medicine can optimize—not merely manage—health.
Is it false to say that if a man in his mid-60s can do this, everyone can? Technically, yes. But it is overwhelmingly true, in the absence of advanced disease, that the majority of people who believe they “can’t” are limited not by age or biology, but by low expectations, lack of knowledge, and the absence of proper training.
The Distraction Problem
Patients, friends, and social media followers are constantly searching for a “Fountain of Youth” in supplements, medications, and laboratory tests. The irony is that this relentless pursuit of shortcuts actively distracts from the only interventions that consistently and reproducibly work.
Social media has amplified this problem. Much of what is marketed as “health” content is misleading or false—and it trains people to chase noise instead of building physiologic capacity.
The purpose of this blog is to redirect attention away from that noise and toward what actually determines long-term health, functional independence, and survival.
The framework presented here is not what U.S. medicine currently offers to most patients, and for many it will create cognitive dissonance. That is intentional. The prevailing U.S. medical model is designed to diagnose and manage disease—not to define, measure, or build health optimization.
For that reason, every position in this blog is grounded in rigorous scientific evidence—not opinion, ideology, or anecdote. This represents a necessary paradigm shift, driven by decades of outcomes-based research showing that cardiorespiratory fitness and skeletal muscle capacity outperform traditional risk markers in predicting long-term health and survival⁽²,⁸,²⁴,²⁶,³⁴,³⁷–³⁹,⁴⁸–⁵¹⁾.
This blog is not a criticism of the treatment of disease with medication or surgery. Rather, it highlights a complementary path—one that is rarely addressed in most U.S. medical offices—focused on building and preserving physiologic capacity to optimize health and achieve the greatest possible longevity.
This blog is about the real “Fountain of Youth.”
What Most People Get Wrong About Health After 40
The internet is filled with misleading or outright false statements about aging, exercise, and what is “safe” or “possible” after 40. If it’s on social media, it is probably wrong—and often designed to sell you something of unproven value.
These myths don’t just confuse people; they cause real harm by lowering expectations, discouraging training intensity, and convincing older adults that decline is inevitable.
Below are two of the most common misconceptions—and the evidence-based corrections.
Myth #1 — “Walking or any movement is good enough.”
Walking is healthy.
But walking alone is rarely sufficient to meaningfully raise VO₂max or preserve skeletal muscle mass with aging.
Step counts and activity rings track movement, not physiologic adaptation. If movement does not impose sufficient intensity or progressive overload, it will not meaningfully improve VO₂max, strength, or long-term health.
VO₂max improves through adequate intensity—most often sustained Zone 2 training… layered with periodic higher-intensity efforts.
Walking is beneficial for mood, joint health, and general well-being—but it is not, by itself, a comprehensive training strategy for preserving physiologic capacity after midlife.
Myth #2 — “Building muscle after 40 is too dangerous.”
False.
Older adults can gain muscle reliably and safely under structured training programs⁽³⁵–³⁹⁾. In many cases, they do so with lower injury rates than younger individuals when programs are appropriately designed and supervised.
The greater danger is the opposite:
Avoiding strength training → frailty → falls → hospitalization → accelerated decline. Strength training is not reckless.
It functions as protective medicine.
Myth #3 — “When my heart rate increases during resistance training, that time counts toward my cardio zone training.”
This is a common and understandable misconception. It is intuitive to think that if heart rate rises during any form of exercise, it must contribute to cardiovascular fitness—since cardiovascular training also requires an elevated heart rate.
But this is incorrect.
Resistance training can raise heart rate—but heart rate elevation alone does not define cardiovascular training, nor does it improve VO₂max in a meaningful way.
Why?
• VO₂max improves through sustained, rhythmic, aerobic demand, where large muscle groups continuously consume oxygen over time
• Resistance training is intermittent by design, consisting of short bursts of effort followed by rest
• During lifting, heart rate rises primarily due to pressure responses, bracing, and sympathetic activation, not sustained oxygen utilization.
• The cardiovascular system is never stressed long enough to trigger the structural adaptations required for VO₂max improvement (e.g., increased stroke volume, capillary density, mitochondrial biogenesis)
In simple terms:
• Lifting trains force production
• Cardio trains oxygen delivery and utilization
• A fast pulse during lifting reflects acute stress, not aerobic conditioning
This distinction matters clinically.
Time spent lifting—even when heart rate is elevated—does not accumulate toward cardio “zone time”, and it does not substitute for deliberate aerobic training. Both systems are essential, but they adapt through fundamentally different mechanisms.
This is why muscle and VO₂max must be trained separately—and intentionally to optimize health.
Hormone Optimization: The Often-Ignored Prerequisite for Training After 50
One reality rarely discussed—yet consistently supported in research—is that many adults over 50 cannot build muscle or improve aerobic capacity effectively without first correcting hormonal deficiencies.
Testosterone and estrogen decline with age, directly impairing:
- Muscle protein synthesis
- Recovery capacity
- Mitochondrial function
- Aerobic performance
- Motivation, drive, and energy
These aren’t “soft symptoms.”
They are measurable physiologic barriers.
This leads to one of the most damaging myths:
“I can’t lift heavy or train intensely because I’m old.”
In reality, many people can’t train intensely because their hormones are too low to support adaptation—not because of age itself.
When supervised appropriately, hormone replacement can help restore the physiologic environment required for:
- Strength training
- Muscle hypertrophy
- VO₂max improvement
- Recovery capacity
- Consistency
HRT does not replace training.
It enables it.
For many women over 50 and many men over 60, HRT is not optional—it is the physiologic prerequisite for meaningful strength and VO₂max adaptation.
If You’re Over 40, You’ve Probably Noticed Something Important
No one is coming to save your health for you.
Your doctor can monitor it—but most are not trained in building or optimizing long-term health.
Your lab work can reflect it.
Your medications can support it.
No modifiable factor protects your health as powerfully as:
- Muscle
- Aerobic fitness (VO₂max)
Both are independently associated with⁽²,⁸⁾:
- Lower all-cause mortality
- Lower cardiovascular risk
- Greater independence
- Better metabolic and brain health
Despite the widespread reliance on laboratory testing to assess health, muscle strength and aerobic fitness (VO₂max) are among the strongest independent predictors of survival ever identified—often outperforming traditional laboratory markers and cardiovascular risk factors.⁽²,⁸⁾
At the Foundation, muscle and VO₂max are the primary determinants of functional longevity—how well you live, not just how long.
Why VO₂max Outperforms Nearly Every Laboratory Marker
Modern medicine indeed places heavy emphasis on blood tests as indicators of health. While these measures are often clinically valuable, most laboratory tests reflect isolated pathways or individual organ systems, not whole-body physiologic capacity.
Metrics such as VO₂max dixer precisely because they require coordinated performance across nearly every major organ system.
To achieve even an average VO₂max, nearly every major organ system must be functioning well, including:
- Cardiovascular system
- Pulmonary system
- Hematologic system
- Musculoskeletal system
- Central and peripheral nervous systems
- Endocrine system
- Renal and hepatic systems
In practice, VO₂max functions as a whole-organism stress test.
If any major system is impaired, VO₂max declines.
This is why VO₂max is so powerfully predictive of survival—and why improving VO₂max often normalizes many laboratory abnormalities, rather than the other way around. This relationship is frequently misunderstood in clinical practice, leading to misplaced priorities in care.
If we have decades of data demonstrating the importance of VO₂max, DEXA-derived body composition, and the preservation of muscle mass for long-term health, a reasonable question follows: why has Western medicine not adopted these measurements—or organized care around what they so clearly predict?
That question matters. The answer is complex, involving structural, cultural, and economic forces. It deserves its own discussion—and lies beyond the scope of this article. It may be addressed in a future piece.
Muscle: The Central Organ of Independence
For those who believe muscle is unimportant or “just vanity,” this must be stated clearly:
Muscle is not just cosmetic.
It is structural, metabolic, and protective.
Why muscle matters after 40, 50, 60, 70, 80, and beyond:
- Improves balance and stability, reducing fall risk⁽⁹⁾
- Preserves mobility and daily function⁽¹⁰⁾
- Stimulates bone remodeling and skeletal integrity⁽¹¹⁾
- Enhances insulin sensitivity and glucose disposal⁽¹²⁾
- Raises resting metabolic rate and metabolic flexibility⁽¹³⁾
- Provides physiologic reserve during illness, injury, or surgery⁽¹⁴⁾
Tendon Health (An Often-Overlooked—and Often Misunderstood—Benefit of Strength Training)
Tendons are living tissue that adapt—slowly—to mechanical loading. With aging and inactivity, they stiffen, thin, lose collagen quality, and become more injury-prone.
Paradoxically, many people believe resistance training should be avoided with age to ‘protect’ tendons. The opposite is true: it is under-loading—not progressive, appropriately dosed loading—that accelerates tendon degeneration. Properly programmed strength training preserves not just muscle, but the muscle–tendon unit, which is essential for force transmission, joint stability, and injury prevention. ⁽¹⁵,¹⁶⁾
Key tendon-specific benefits of resistance training
- Preserves tendon stiffness and elasticity, improving force transfer and movement efficiency⁽¹⁵⁾
- Reduces the risk of tendon rupture and overuse injury, particularly in the Achilles, patellar, and rotator cuff tendons⁽¹⁶⁾
- Improves rate of force development, critical for balance recovery and fall prevention⁽¹⁷⁾
- Maintains joint stability under load, reducing compensatory movement and arthritis progression⁽¹⁸⁾
- Supports power and deceleration—not just strength—essential for stair climbing, rising from chairs, and fall prevention⁽¹⁹⁾
Like VO₂max, muscle represents physiologic capacity.
Within physiologic limits, there is no upper “normal” threshold—greater capacity confers greater resilience.
Muscle Metrics We Track at the Foundation
Grip strength, commonly used in research and some medical practices, is simple and predictive at a population level. However, for individuals over 40, we think it poorly captures the traits that most strongly determine independence and real-world function.
At the Foundation, we therefore favor age- and sex-normalized, whole-body functional strength measures that better reflect true physiologic capacity.
Foundation Functional Strength Index (FSI)
We begin with DEXA-derived appendicular lean mass (ALM), indexed to height².
DEXA scan derived ALM/ht² is one of the most extensively validated measures of skeletal muscle mass and has been used for over two decades to define sarcopenia and predict disability, frailty, and mortality⁽⁴¹–⁴⁴⁾.
Major international consensus groups—including the European Working Group on Sarcopenia in Older People (EWGSOP2) and Asian Working Group for Sarcopenia (AWGS)—recognize DXA scan measured ALM/ht² as a standard method for quantifying muscle mass in aging populations⁽⁴⁵–⁴⁷⁾.
BMI and scale weight provide little insight into aging physiology. In contrast, ALM/ht² directly measures skeletal muscle, making it vastly superior for assessing frailty risk, functional capacity, and long-term health outcomes.
Physiologic Capacity: Performance Contextualization
Physiologic capacity is best interpreted in context. Individual performance is therefore evaluated relative to age- and sex-specific normative distributions derived from large population datasets.
Percentile rankings for aerobic fitness (VO₂max) are based on established normative tables from the Cooper Institute and are referenced by the American College of Sports Medicine (ACSM)⁽⁴⁸⁾. Additional population-level reference values are available from large national datasets, including Canadian health surveys, which report age- and sex-specific percentiles for cardiorespiratory fitness⁽⁴⁹⁾. Together, these sources allow aerobic capacity to be meaningfully contextualized relative to demographic peers.
To complement DEXA-derived appendicular lean mass (ALM), we incorporate a three-movement functional strength battery assessing whole-body force production and transfer:
- Push-ups — upper-body and trunk strength
- Air squats — lower-body strength, coordination, and power
- Knee-bent, unanchored sit-ups — trunk endurance and force transmission
We use knee-bent, unanchored sit-ups rather than curl-ups because they assess functional trunk strength through a full range of motion that more closely reflects real-world tasks, including rising from the floor and maintaining independence with aging. Variants of this test have also been used for decades by the U.S. military as a practical, scalable measure of trunk strength and conditioning.
Performance Targets After 40
- Minimum target: ≥75th percentile for age and sex
- Ideal Foundation goal: ≥90th percentile
- See FSI Bands below to understand where you sit
1. Push-ups
Protocol (Men & Women)
Begin in a plank position with hands under shoulders, body in a straight line from head to heels (men) or head to knees (women). Lower the body until the chest approaches the floor, then press back to full elbow extension. Perform repetitions at a controlled cadence (~2 seconds down, ~2 seconds up) without sagging, piking, or using momentum.
Continue until fatigue or loss of proper form; there is no time limit. Score is the total number of technically valid repetitions.

2.Air squats Protocol
Stand with feet shoulder-width apart, toes slightly out, weight mid-foot. With arms crossed or held forward, descend to at least knee-level depth and return to full standing. Perform repetitions at a controlled cadence (~2 seconds down, ~2 seconds up) with heels on the floor and knees tracking over toes. Continue until fatigue or loss of proper form; there is no time limit. Score is the total number of technically valid repetitions.
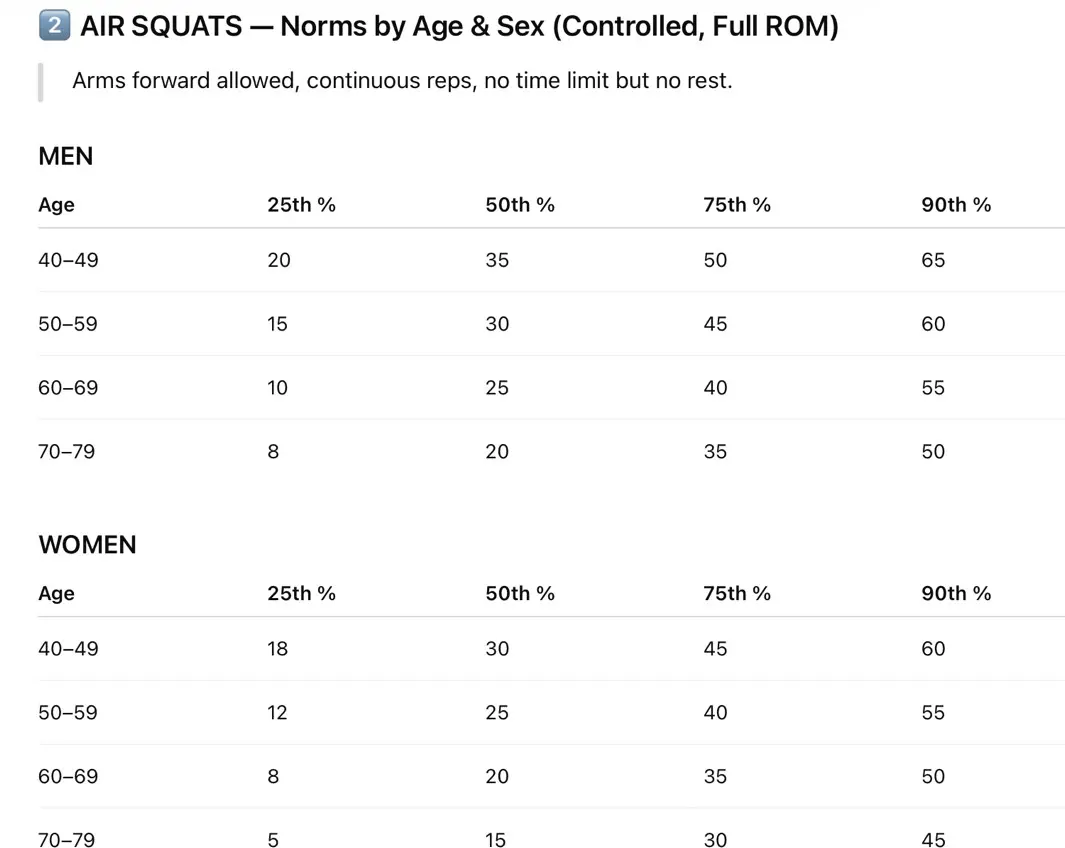
3.Knee-bent, unanchored sit-ups
Protocol: Knee-bent, unanchored sit-ups are performed at a controlled cadence of ~2 seconds up and ~2 seconds down, continuing until volitional fatigue or loss of proper form, with no preset time limit.


These metrics reflect physiologic capacity—not appearance.
The Synergy: Why Muscle + VO₂max Change Everything
Optimizing muscle or aerobic capacity in isolation is beneficial. Optimizing both changes the trajectory of aging.
Skeletal muscle and VO₂max address the two dominant, independent pathways of age-related decline: loss of functional capacity and loss of physiologic reserve. Together, they define physiologic resilience—the ability to tolerate stress, recover efficiently, and maintain independence across illness, injury, and aging.
After midlife, this combined capacity becomes the primary determinant of how well—and how long—people remain independent.
Conclusion
I am often asked—usually in the name of efficiency—which matters more: improving VO₂max or building muscle. Unfortunately, the premise is flawed. These are not competing priorities; they are complementary systems that function together. Optimal health requires both.
In a public interview, Dr. Mehmet Oz once answered that the most important factor for good health was “exercise.” That answer is directionally correct—but incomplete. What matters is which exercise, why, and what it builds.
If I had to end this blog with two sentences, they would be these:
Muscle protects your independence⁽⁸⁾. VO₂max protects your survival⁽²⁾.
Together, they redefine what life after 40 can look like—more powerfully than any laboratory test, imaging study, or genetic report ever can.
Aging well is not accidental. It is strategic, deliberate, and earned. It requires a written plan, objective measurement, and regular follow-up—just as any serious medical intervention would.
These are the two pillars of health optimization in the second half of life—not supplements, not medications and not wishful thinking.
Neglect them, and the trajectory is predictable: functional capacity declines, physiologic reserve erodes, illness arrives earlier, recovery worsens, and death occurs sooner than biology would otherwise dictate.
No drug can fully replace lost muscle or a failing aerobic engine once they are gone.
Author
Jonathan A. Jarman, MD — Yale–NYU trained physician, honored for outstanding USMLE Board performance (top 1% Psychiatry, top 10% Biochemistry); engaged in health-optimization and longevity research; founder of the Julian A. Jarman MD Research Foundation.
References
1.Peterson MD, Sen A, Gordon PM. Influence of resistance exercise on lean body mass in aging adults: a meta-analysis. Med Sci Sports Exerc. 2011;43(2):249-258.
→ Meta-analysis showing older adults reliably gain lean mass with resistance training.
2.Laukkanen JA, Kunutsor SK, Yates T, et al. Cardiorespiratory fitness and all-cause mortality. Mayo Clin Proc.2018;93(12):1701-1711.
→ Higher VO₂max strongly and dose-dependently predicts lower all-cause mortality.
3.Kane GC, Karon BL, Mahoney DW, et al. Progressive diastolic dysfunction and risk of heart failure. 2011;306(8):856-863.
→ Grade I diastolic dysfunction is common with aging and prognostically meaningful.
4.Plews DJ, Laursen PB, Stanley J, et Training adaptation and heart rate variability. Eur J Appl Physiol.2013;113(7):1651-1659.
→ HRV is a valid tool for monitoring training readiness and recovery.
5.Haykowsky MJ, Brubaker PH, John JM, et Determinants of exercise intolerance in HFpEF. J Am Coll Cardiol.2011;58(3):265-274.
→ Endurance training improves diastolic function and exercise capacity.
6.Joyner MJ, Coyle EF. Endurance exercise performance: physiology of champions. J Physiol. 2008;586(1):35-44.
→ VO₂max reflects integrated cardiac, pulmonary, muscular, and metabolic function.
7.Arena R, Myers J, Williams MA, et Assessment of functional capacity. Circulation. 2007;116(3):329-343.
→ VO₂max and GLS together provide powerful prognostic cardiac assessment.
8.Ruiz JR, Sui X, Lobelo F, et al. Association between muscular strength and mortality. 2008;337:a439.
→ Muscular strength independently predicts lower all-cause mortality.
9.Sherrington C, Fairhall NJ, Wallbank GK, et al. Exercise for preventing falls. Br J Sports Med. 2020;54(15):885-891.
→ Strength and power training significantly reduce fall risk in older adults.
10.Studenski S, Perera S, Patel K, et Gait speed and survival. JAMA. 2011;305(1):50-58.
→ Functional performance reflects global physiologic reserve and survival.
11.Kohrt WM, Bloomfield SA, Little KD, et Physical activity and bone health. Med Sci Sports Exerc.2004;36(11):1985-1996.
→ Mechanical loading is essential for bone remodeling and skeletal integrity.
12.Hawley JA, Lessard SJ. Exercise training and insulin action. J Appl Physiol. 2008;104(3):775-781.
→ Skeletal muscle adaptations drive improved insulin sensitivity.
13.Wolfe RR. The underappreciated role of muscle in health and disease. Am J Clin Nutr. 2006;84(3):475-482.
→ Muscle functions as a central metabolic and protective organ.
14.Cawthon PM, Fox KM, Gandra SR, et Muscle and hospitalization risk. J Gerontol A Biol Sci Med Sci.2009;64A(6):658-664.
→ Low muscle mass and strength predict hospitalization and poor outcomes.
15.Magnusson SP, Langberg H, Kjaer Pathogenesis of tendinopathy. Nat Rev Rheumatol. 2010;6(5):262-268.
→ Tendons degenerate with under-loading, not appropriately dosed loading.
16.Bohm S, Mersmann F, Arampatzis A. Tendon adaptation to mechanical loading. Sports Med. 2015;45(4):459-478.
→ Progressive resistance training preserves tendon structure and stiffness.
17.Maffiuletti NA, Aagaard P, Blazevich AJ, et Rate of force development. Eur J Appl Physiol. 2016;116(6):1091-1116.
→ Power and force development are critical for balance and fall prevention.
18.Sharma Osteoarthritis of the knee. N Engl J Med. 2021;384:51-59.
→ Muscle strength improves joint stability and slows functional decline.
19.Reid KF, Fielding RA. Skeletal muscle power in aging. Exerc Sport Sci Rev. 2012;40(1):4-
→ Muscle power is a key determinant of independence in older adults.
24.Blair SN, Kohl HW, Paffenbarger RS Jr, et al. Physical fitness and mortality. 1989;262(17):2395-2401.
→ Low fitness is a stronger mortality predictor than many traditional risk factors.
25.Fragala MS, Cadore EL, Dorgo S, et al. Resistance training for older adults. J Strength Cond Res. 2019;33(8):2019-2052.
→ Resistance training is safe and effective across advanced age groups.
26.Kodama S, Saito K, Tanaka S, et al. Fitness and mortality meta-analysis. 2009;301(19):2024-2035.
→ VO₂max shows graded, inverse association with mortality.
24.Ross R, Blair SN, Arena R, et al. Fitness as a clinical vital sign. Circulation. 2016;134(24):e653-e699.
→ Cardiorespiratory fitness should be routinely assessed in clinical practice.
35–39.Peterson MD et al.; Fiatarone MA et al.; Borde R et al.; Liu CJ, Latham NK; Westcott WL.
→ Multiple trials confirm strength training is safe, effective, and protective in older adults.
41–44.Baumgartner RN et al.; Newman AB et al.; Studenski SA et al.; Cruz-Jentoft AJ et al.
→ DXA-derived ALM/ht² predicts frailty, disability, and mortality.
45.Cruz-Jentoft AJ, Bahat G, Bauer J, et al. EWGSOP2 consensus. Age Ageing. 2019;48(1):16-31.
→ European consensus defining sarcopenia using DXA-based lean mass.
46.Chen LK, Woo J, Assantachai P, et al. AWGS consensus update. J Am Med Dir Assoc. 2020;21(3):300-307.
→ Asian consensus recognizing DXA ALM/ht² as standard muscle metric.
47.Shafiee G, Keshtkar A, Soltani A, et al. Sarcopenia prevalence worldwide. Osteoporos Int. 2017;28(6):1813-1825.
→ Sarcopenia prevalence rises sharply with age and predicts adverse outcomes.
48.Kaminsky LA, Arena R, Myers J. CRF reference standards. Mayo Clin Proc. 2015;90(11):1515-1523.
→ Provides age- and sex-specific VO₂max percentile norms.
49.Lang JJ, Tomkinson GR, Janssen I, et al. Fitness surveillance. Sports Med. 2018;48(11):2577-2590.
→ Population VO₂max percentiles strongly associate with health outcomes.
50–51.Myers J et al. N Engl J Med. 2002; Kokkinos P et al. Circulation. 2010.
→ Exercise capacity outperforms traditional cardiovascular risk factors for survival.
Health Blog #20 - Nandrolone Therapy in Testosterone Replacement Therapy (TRT): Benefits, Risks & Safety
Nandrolone Therapy in Testosterone Replacement Therapy (TRT): Benefits, Risks & Safety
This evidence-based review focuses specifically on medically supervised low-dose nandrolone therapy and does not address supraphysiologic anabolic steroid abuse.
Nandrolone therapy refers to the medically supervised use of nandrolone decanoate, typically at low doses (50–100 mg weekly), as an adjunct to testosterone replacement therapy (TRT) to support muscle preservation and anabolic signaling. In carefully selected patients, low-dose nandrolone may be added to optimized TRT to enhance lean mass and functional strength while maintaining biomarker-defined safety parameters.
Many patients searching “is nandrolone safe?”, “nandrolone vs testosterone,” or “Deca with TRT” are trying to determine whether adjunct therapy can improve muscle mass without increasing cardiovascular or prostate risk.
By Jonathan A. Jarman, MD
Yale-trained, board-certified physician and founder of the Julian A. Jarman MD Research Foundation.
Background and Pharmacology
Nandrolone decanoate (commonly known by the brand name Deca-Durabolin) is an injectable anabolic-androgenic steroid (AAS) derived from testosterone.¹ It is one of several synthetic derivatives developed during early efforts to refine androgen therapy and better distinguish anabolic from androgenic effects.
In simple terms:
- Anabolic refers to tissue-building effects, particularly increases in muscle and bone mass.
- Androgenic refers to masculinizing effects, such as facial and body hair growth, voice deepening, prostate stimulation, and skin changes.
Nandrolone is present naturally in men in very small amounts as a minor byproduct of steroid metabolism, although circulating levels are far lower than those of testosterone.² Early anti-doping testing identified trace endogenous nandrolone metabolites, leading to refinements in detection thresholds.³
Nandrolone was developed in the late 1950s and introduced into clinical medicine in the early 1960s, typically at doses of 50–100 mg weekly.¹ It has been used historically in conditions associated with catabolic stress such as anemia, osteoporosis, severe burns, chronic illness-related weight loss, and muscle wasting.⁴
Historical prescribing information reflects these traditional dosing ranges, as outlined in the FDA labeling for nandrolone decanoate.
FDA prescribing information for nandrolone decanoate is available through the U.S. Food and Drug Administration database.
Structurally, nandrolone differs from testosterone by the absence of the C19 methyl group (“19-nortestosterone”).¹ This modification alters tissue interactions and is associated with a higher anabolic-to-androgenic activity ratio in animal models.¹,⁹
Concerns about nandrolone largely stem from misuse in athletic and bodybuilding settings at very high doses (often 400–1200 mg weekly) without medical supervision.⁶
Nandrolone vs Testosterone: Metabolism and Tissue Effects
Although nandrolone is derived from testosterone, it behaves differently in human tissues.¹,⁹
Testosterone converts to:
- Dihydrotestosterone (DHT) via 5-alpha reductase
- Estradiol via aromatase
DHT strongly stimulates androgen-sensitive tissues such as prostate and skin but does not appear to significantly contribute to skeletal muscle hypertrophy in humans.⁵
Nandrolone also undergoes 5-alpha reduction, but its reduced metabolite (DHN) is less androgenic than DHT.¹,⁹ It aromatizes to estrogen, generally to a lesser extent than testosterone.¹,⁹
Because of these differences, nandrolone has historically been described as having a relatively higher anabolic-to-androgenic ratio.¹,⁹ Much of this distinction, however, comes from animal and laboratory data rather than long-term outcome studies in aging men.⁸
Comparative Overview
| Feature | Testosterone | Nandrolone |
| 5-alpha reduction | To DHT | To DHN (less androgenic) |
| Aromatization | Yes | Yes (less) |
| Anabolic-to-androgenic ratio | 1:1 reference | 11:1 (animal data) |
| Prostate stimulation | Higher (via DHT) | Lower 5α-reduced activity |
| Clinical role | Primary TRT | Adjunct in selected TRT cases |
In summary, testosterone remains primary hormone replacement therapy, while physiologic nandrolone is considered selectively as adjunct anabolic support.
The 11:1 Anabolic-to-Androgenic Ratio Explained
The 11:1 ratio does not mean nandrolone is eleven times more anabolic than testosterone.¹,⁹
The ratio derives from rodent bioassays measuring relative muscle versus prostate stimulation.¹,⁹ In those models, nandrolone demonstrated approximately 1.5–3 times greater anabolic activity in skeletal muscle with comparatively less prostate stimulation.¹,⁹
These findings are:
- Dose-dependent
- Model-dependent
- Not directly extrapolatable to clinical dosing in humans
As nandrolone dose increases, anabolic signaling increases, but the relationship is nonlinear and accompanied by escalating risk.
In humans, resistance training itself is anabolic, and mechanical loading and androgen signaling act synergistically.¹⁰ This interaction likely explains why nandrolone may provide meaningful additional anabolic support when combined with optimized testosterone therapy and structured training.
Potential Benefits of Low-Dose Nandrolone Therapy
At medical doses in selected patients, nandrolone supports:
- Increased lean body mass¹,⁹
- Improved nitrogen retention¹,⁹
- Enhanced strength when combined with resistance training¹⁰
- Bone density support in selected individuals⁴
- Preservation of muscle mass in catabolic states⁴
Some patients report improvement in joint discomfort. Proposed mechanisms include enhanced collagen synthesis and connective tissue hydration.¹¹ However, controlled data in aging men are limited, and this should not be considered a proven therapeutic indication.⁸
Low-dose nandrolone has been discussed in age-related muscle loss (sarcopenia) when testosterone alone does not fully restore lean mass.
Evidence: What We Know and What Remains Uncertain
What We Know
- Nandrolone increases lean body mass in a dose-dependent manner.¹,⁹
- It has decades of historical medical use in catabolic conditions.⁴
- Most severe adverse effects in the literature involve supraphysiologic misuse.⁶
What Remains Uncertain
- Long-term cardiovascular outcomes of combined testosterone + nandrolone therapy
- Long-term prostate outcomes
- Optimal duration of adjunct therapy
Although nandrolone has a long history of medical use, robust long-term outcome trials in aging men receiving combination therapy remain limited.
Risks and Side Effects of Nandrolone Therapy
Like all anabolic-androgenic hormones, nandrolone carries potential risks.⁶ These risks are dose-dependent and significantly more common at supraphysiologic doses used in athletic misuse.⁶
Potential concerns include:
- Increased hematocrit⁶
- Changes in lipid parameters (lower HDL, potential ApoB elevation)⁶
- Blood pressure elevation⁶
- Fluid retention⁶
- Estrogen-related effects¹
- Prolactin elevation⁷
- Suppression of endogenous hormone production⁷
Cardiovascular risk appears mediated primarily through measurable variables such as hematocrit, ApoB, blood pressure, and fluid status.⁶ When these biomarkers are carefully monitored and maintained within healthy ranges, theoretical risk should be mitigated.⁸
Monitoring Framework for Nandrolone Therapy
Baseline & Metabolic Assessment
To establish cardiometabolic risk and define objective endpoints.
- Liver enzymes
• HbA1c or fasting glucose
• hs-CRP
• DEXA scan
Hematologic Monitoring
To detect erythrocytosis and reduce viscosity-related risk.³
- Complete blood count
Lipid & Cardiovascular Markers
To assess atherogenic burden and hemodynamic response.⁴⁵
- Lipid panel (including ApoB)
• Blood pressure
Cardiac Structural & Functional Assessment
To detect subclinical ventricular remodeling or impaired myocardial mechanics.⁶⁷
- Baseline transthoracic echocardiogram
• Global Longitudinal Strain (GLS)
• Repeat imaging at defined interval if therapy continues long-term
Hormonal Assessment
To confirm physiologic dosing and endocrine stability.
- Total testosterone via LC/MS¹²
• Estradiol
• SHBG
• DHT
• Prolactin
Prostate Surveillance
To monitor androgen-sensitive tissue response.⁸
- PSA
Clinical Assessment
To correlate laboratory data with functional response.
- Symptom review (energy, strength, libido, mood, fluid retention, joint symptoms)
Because long-term human data on low-dose nandrolone are limited, cardiac imaging is included as a precautionary measure. Global Longitudinal Strain (GLS) provides a sensitive marker of myocardial function and may detect early mechanical changes before reductions in ejection fraction occur. The goal is surveillance, not presumption of harm.
Distinguishing Medical Therapy from Athletic Misuse
Supervised medical dosing of nandrolone (50–100 mg weekly) differs fundamentally from supraphysiologic anabolic steroid use in athletic settings.
Most published reports describing severe lipid abnormalities, cardiovascular strain, mood instability, and endocrine disruption involves:
- Doses of 400–1200 mg weekly
- Stacking with multiple agents
- Lack of structured laboratory monitoring
- Extended unsupervised use⁶
These represent a different exposure pattern and risk profile from conservative, physician-guided adjunct therapy.
This distinction does not eliminate risk at medical doses but is essential for accurate interpretation of the literature.
When Nandrolone May Be Considered
Nandrolone is not routine TRT.
It may be considered selectively in patients with:
- Sarcopenia
- Lean mass inadequacy despite optimized TRT
- Catabolic stress states
- Bone density concerns
The purpose is enhancement of anabolic signaling — not supraphysiologic hormone levels.
Supraphysiologic nandrolone levels are being studied.
Foundation Clinical Approach
Key principles include:
- Conservative dosing unless part of a study
- Structured laboratory monitoring
- Cardiovascular risk management
- Ongoing reassessment
- Discontinuation if benefit not demonstrated
Who Should Not Consider Nandrolone Therapy?
Contraindications include:
- Uncontrolled polycythemia
- Severe untreated dyslipidemia
- Active prostate cancer
- Poorly controlled cardiovascular risk
- Inability to undergo monitoring
Clinical Takeaway
Medically supervised adjunct nandrolone therapy provides additional anabolic support in carefully selected men receiving optimized testosterone therapy. Biomarker monitoring is essential. Long-term outcome data remain limited.
All treatment decisions regarding nandrolone therapy should be made through an informed discussion with a physician experienced in hormone therapy and the clinical use of nandrolone.
FAQs
Is nandrolone stronger than testosterone?
Nandrolone has a higher anabolic-to-androgenic ratio in animal models. This reflects relative tissue selectivity rather than absolute muscle-building potency, i.e. animals don’t train! Its clinical effects depend on dose, metabolism, training stimulus, protein intake and patient context.
Is nandrolone safe when used with testosterone therapy?
At medical doses with structured monitoring, risks may be mitigated. However, long-term outcome data remain limited.
Why is nandrolone controversial?
Most controversy stems from high-dose athletic misuse rather than physician-supervised low-dose therapy.
Jonathan A. Jarman, MD is a Yale-trained, board-certified physician with clinical experience in hormone and performance physiology. His work focuses on the physiology of high-performance aging, including VO₂max, muscle strength, autonomic regulation, emotional control, and cognitive resilience. He leads the Julian A. Jarman MD Research Foundation, which supports and advances research in these domains.
Last updated: Feb 2026
References:
- Kicman AT. Pharmacology of anabolic steroids. Br J Pharmacol. 2008;154(3):502-521. doi:10.1038/bjp.2008.165
- Reznik Y, Dehennin L, Coffin C, Mahoudeau J. Urinary nandrolone metabolites in male subjects: endogenous origin. Clin Endocrinol (Oxf). 2001;55(4):533-539. doi:10.1046/j.1365-2265.2001.01363.x
- Dehennin L, Lafarge P, Peres G, Lafarge JP. Endogenous origin of 19-norandrosterone in human urine: implications for doping control. J Chromatogr B Biomed Sci Appl. 1999;687(1):85-91. doi:10.1016/S0378-4347(98)00458-2
- Basaria S. Androgen abuse in athletes: detection and consequences. J Clin Endocrinol Metab. 2010;95(4):1533-1543. doi:10.1210/jc.2009-1579
- Handelsman DJ. Androgen physiology, pharmacology, use and misuse. Endocr Rev. 2013;34(3):341-375. doi:10.1210/er.2012-1036
- Hartgens F, Kuipers H. Effects of androgenic-anabolic steroids in athletes. Sports Med. 2004;34(8):513-554. doi:10.2165/00007256-200434080-00003
- Turek PJ, Williams RH, Gilbaugh JH 3rd, Lipshultz LI. The reversibility of anabolic steroid–induced azoospermia. J Urol. 1995;153(5):1628-1630. doi:10.1016/S0022-5347(01)67345-5
- Bhasin S, Brito JP, Cunningham GR, et al. Testosterone therapy in men with hypogonadism: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2018;103(5):1715-1744. doi:10.1210/jc.2018-00229
- Pan MM, Kovac JR. Beyond testosterone cypionate: evidence behind the use of nandrolone in male health and wellness. Transl Androl Urol. 2016;5(2):213-219. doi:10.21037/tau.2016.03.03
- Bhasin S, Storer TW, Berman N, et al. The effects of supraphysiologic doses of testosterone on muscle size and strength in normal men. N Engl J Med. 1996;335(1):1-7. doi:10.1056/NEJM199607043350101
- Wood TO, Cooke PH, Goodship AE. Effects of anabolic steroids on tendon. J Bone Joint Surg Br.1988;70(3):383-386.
- Bachman E, Feng R, Travison T, et al. Testosterone induces erythrocytosis via increased erythropoietin and suppressed hepcidin: evidence for a new erythropoietin/hemoglobin set point. J Gerontol A Biol Sci Med Sci.2014;69(6):725-735. doi:10.1093/gerona/glt154
- Sniderman AD, Williams K, Contois JH, et al. A meta-analysis of low-density lipoprotein cholesterol, non–high-density lipoprotein cholesterol, and apolipoprotein B as markers of cardiovascular risk. JAMA. 2003;290(1):81-87. doi:10.1001/jama.290.1.81
- Baggish AL, Weiner RB, Kanayama G, et al. Long-term anabolic-androgenic steroid use is associated with left ventricular dysfunction. Circulation. 2010;122(8):804-811. doi:10.1161/CIRCULATIONAHA.109.931063
- Kalam K, Otahal P, Marwick TH. Prognostic implications of global left ventricular dysfunction: a systematic review and meta-analysis of global longitudinal strain and ejection fraction. J Am Coll Cardiol. 2014;63(5):407-416. doi:10.1016/j.jacc.2013.09.043
Taieb J, Mathian B, Millot F, et al. Testosterone measured by 10 immunoassays and by isotope-dilution gas chromatography–mass spectrometry in sera from 116 men, women, and children. Clin Chem. 2003;49(8):1381-1395. doi:10.1373/49.8.1381
About the Author
Jonathan A. Jarman, MD — Yale–NYU trained physician, honored for outstanding USMLE Board performance (top 1% Psychiatry, top 10% Biochemistry); engaged in health-optimization and longevity research; founder of the Julian A. Jarman MD Research Foundation.
